Contents
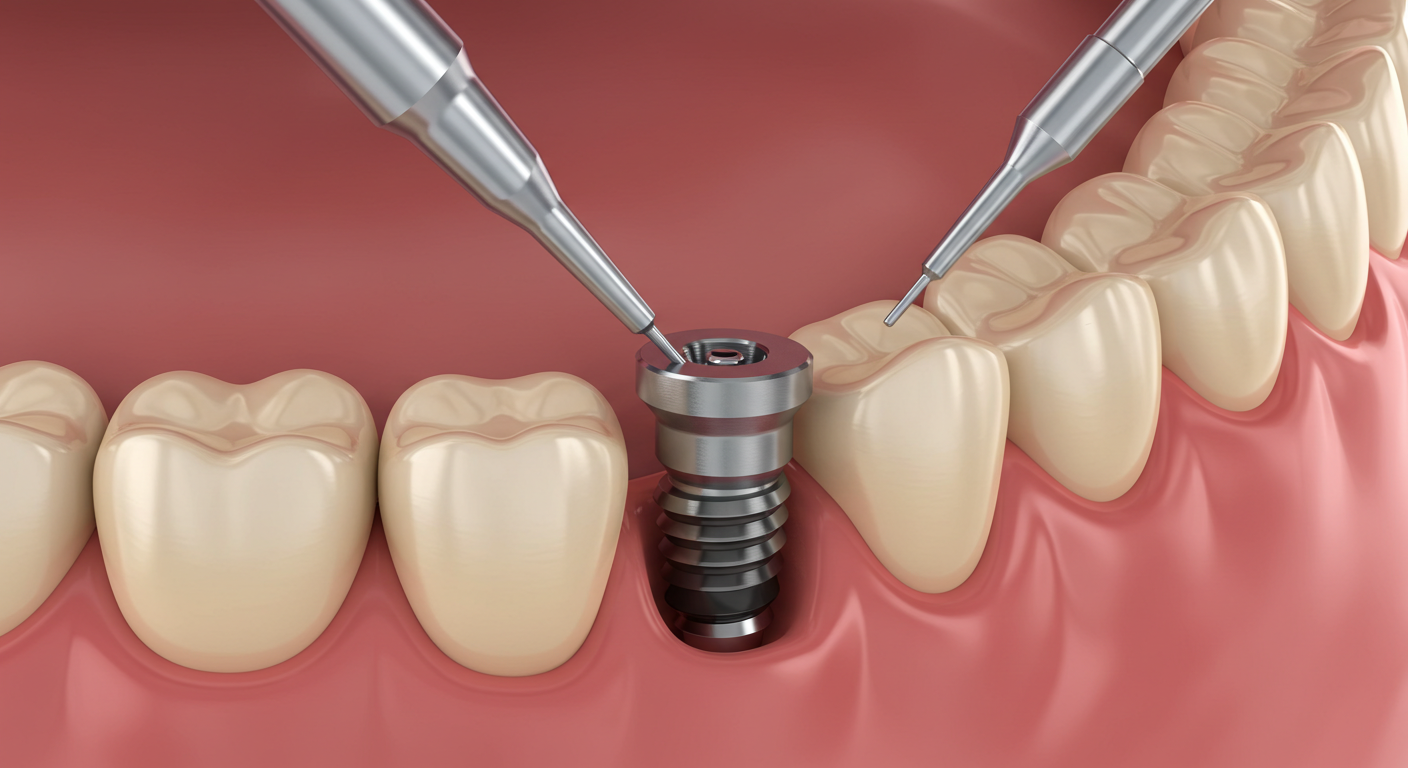
Dental Implant Surgery in 2026: Procedure, Recovery, Costs & Expert Advice
Dental implant surgery is a remarkably predictable procedure that has transformed the lives of millions of patients worldwide. In 2026, advances in digital planning, guided surgical protocols, and accelerated-healing implant surfaces have made the experience faster, more comfortable, and more precise than at any point in the technology's five-decade history. Whether you are facing your first implant placement or considering a full-mouth reconstruction, this guide walks you through every phase of the surgical journey -- from your initial consultation through final restoration.
Understanding Dental Implant Surgery in 2026
At its core, dental implant surgery involves placing a biocompatible post into the jawbone to replace a missing tooth root. The implant is typically made from Grade 4 titanium or, increasingly, from yttria-stabilized zirconia. Once placed, the implant undergoes osseointegration -- a biological process in which living bone tissue grows directly onto the implant surface, locking it securely into the jaw. This integration period, which ranges from 8 to 16 weeks depending on bone quality and implant surface technology, is what gives dental implants their remarkable stability and longevity.
Modern implant surgery in 2026 benefits from several technological leaps. Cone-beam computed tomography (CBCT) provides sub-millimeter 3D imaging of the jaw, allowing surgeons to map bone density, nerve canals, and sinus floors before making a single incision. Digital surgical guides, 3D-printed from this imaging data, translate the virtual plan into the patient's mouth with precision measured in fractions of a millimeter. The result is shorter surgeries, smaller incisions, and faster recovery.
Pre-Surgical Evaluation: Are You a Candidate?
Not every patient is an immediate candidate for implant surgery. A thorough pre-surgical evaluation determines whether placement can proceed directly or whether preparatory procedures are needed first. Your surgeon will assess:
- Bone volume and density: A CBCT scan reveals whether there is enough bone height, width, and density to support an implant. If not, bone grafting may be required.
- Gum health: Active periodontal disease must be treated and stabilized before implant placement.
- Medical history: Conditions such as uncontrolled diabetes, active cancer treatment, recent bisphosphonate use, or immunosuppressive therapy can affect healing and may be contraindications.
- Smoking status: Smoking significantly impairs blood supply to healing tissues. Most surgeons require patients to quit at least 4-6 weeks before and after surgery.
- Medications: Blood thinners, certain osteoporosis drugs, and steroids may need to be managed in coordination with your physician.
The Surgical Procedure: What Happens Step by Step
The implant placement appointment itself is typically completed in 30 to 90 minutes per implant, depending on complexity. Here is the standard sequence:
- Anesthesia administration: Local anesthesia numbs the surgical site completely. Patients who experience dental anxiety can opt for oral sedation, IV sedation, or, in rare cases, general anesthesia.
- Incision and flap elevation: The surgeon makes a small incision in the gum tissue and gently reflects the tissue to expose the underlying bone. In minimally invasive (flapless) procedures, a small tissue punch replaces the traditional incision.
- Osteotomy preparation: A series of precision drills, used at controlled speeds with copious saline irrigation to prevent heat damage, create a channel in the bone that matches the implant's diameter and length.
- Implant insertion: The implant is threaded into the prepared site using a torque-controlled handpiece. The surgeon measures the insertion torque -- a value above 35 Ncm generally indicates good primary stability.
- Closure: The gum tissue is repositioned and sutured. In a two-stage protocol, the implant is completely covered by tissue. In a one-stage protocol, a healing abutment protrudes slightly through the gum.
Guided Surgery vs. Freehand Placement
Guided surgery uses a 3D-printed template (surgical guide) that snaps onto adjacent teeth or the ridge, directing the drill path exactly as planned on the computer. This approach is especially valuable for complex cases, immediate-loading protocols, and full-arch restorations. Freehand placement, while still widely practiced by experienced surgeons, relies more heavily on the clinician's skill and intraoperative judgment.
| Feature | Guided Surgery | Freehand Surgery |
|---|---|---|
| Accuracy | Within 0.5-1.0 mm of planned position | Within 1.5-2.5 mm of planned position |
| Surgery Time | Typically 20-40% shorter | Standard duration |
| Incision Size | Often flapless (no incision) | Traditional flap required |
| Additional Cost | $300-$600 for guide fabrication | No additional cost |
| Best For | Complex cases, full-arch, immediate load | Simple single-tooth cases |
Sedation and Anesthesia Options
Most implant surgeries are performed comfortably under local anesthesia alone. However, several sedation options exist for patients with dental anxiety or those undergoing lengthy procedures:
- Nitrous oxide (laughing gas): Mild sedation, wears off within minutes, no driver needed.
- Oral sedation: A prescription pill taken before the appointment produces moderate relaxation. A driver is required.
- IV sedation: Administered by the surgeon or a dental anesthesiologist, provides deeper sedation with rapid onset and adjustable depth. A driver is required.
- General anesthesia: Reserved for highly complex cases or patients who cannot tolerate in-office sedation. Performed in a hospital or surgical center.
Recovery Timeline and Post-Operative Care
Recovery from implant surgery is typically less discomfort-intensive than patients anticipate. Here is a general timeline:
- Days 1-3: Mild to moderate swelling peaks around 48 hours. Ice packs and prescribed or over-the-counter anti-inflammatories manage discomfort effectively. Stick to soft, cool foods.
- Days 4-7: Swelling subsides. Most patients return to normal activities. Avoid chewing directly on the surgical site.
- Weeks 2-3: Sutures dissolve or are removed. The soft tissue around the implant begins to mature.
- Months 2-4: Osseointegration progresses. The implant should not be loaded with biting forces during this critical phase unless an immediate-load protocol was used.
- Months 4-6: The surgeon verifies integration, and the restorative phase (abutment and crown placement) begins.
"The single most important thing a patient can do after implant surgery is follow their post-operative instructions precisely. That means no smoking, no drinking through straws, gentle rinsing with saltwater, and showing up for all follow-up appointments. Compliance with these simple steps dramatically reduces the risk of complications." -- Dr. Sarah Kim, DDS, MS, Board-Certified Oral Surgeon
Complications: What Can Go Wrong and How to Prevent It
The overall complication rate for dental implant surgery is low, but patients should be aware of the possibilities:
- Infection (peri-implantitis): Bacterial colonization around the implant can lead to bone loss if untreated. Incidence is approximately 5-8% at 5 years. Prevention centers on excellent oral hygiene and regular professional maintenance.
- Implant failure: Failure of osseointegration occurs in about 2-4% of cases. Risk factors include smoking, uncontrolled diabetes, and premature loading.
- Nerve injury: Damage to the inferior alveolar nerve during lower-jaw placement can cause numbness or tingling. With CBCT-guided planning, this complication is exceedingly rare.
- Sinus perforation: Upper-jaw implants placed too close to the sinus floor may breach the sinus membrane. This is typically manageable during surgery.
Bone Grafting and Sinus Lifts: When Extra Surgery Is Needed
Approximately 40-50% of implant patients require some form of bone augmentation before or during implant placement. The most common procedures are:
| Procedure | Purpose | Healing Time | Cost Range (2026) |
|---|---|---|---|
| Socket Preservation Graft | Fills the extraction socket to prevent bone collapse | 3-4 months | $500 - $1,200 |
| Lateral Ridge Augmentation | Widens a narrow ridge to support a wider implant | 4-6 months | $1,500 - $3,500 |
| Sinus Lift (Lateral Approach) | Elevates sinus floor to create bone height in upper jaw | 6-9 months | $2,000 - $4,000 |
| Sinus Lift (Crestal Approach) | Less invasive sinus elevation done at time of implant placement | Concurrent with implant healing | $800 - $2,000 |
Implant Surgery Costs and Insurance in 2026
The surgical component of implant treatment -- not including the final crown -- typically costs $1,800 to $3,500 per implant in 2026. This includes the CBCT scan, surgical planning, the implant fixture, the surgery itself, and post-operative follow-up visits. When the abutment and crown are added, the total per-tooth cost rises to $3,500-$6,500.
Dental insurance coverage for implant surgery has expanded in recent years. In 2026, roughly 65% of employer-sponsored PPO plans include some level of implant coverage, up from about 50% in 2022. Coverage typically falls under the "Major Services" category at a 50% coinsurance rate, subject to the plan's annual maximum. Since most annual maximums cap at $1,500-$2,500, insurance often covers only a fraction of the total implant cost.
"I always advise patients to look at the big picture. Yes, the upfront cost of implant surgery exceeds that of a bridge or denture. But when you factor in the longevity of implants, the preservation of adjacent teeth, and the prevention of bone loss, implants are frequently the most cost-effective solution over a 20-year horizon." -- Dr. James Park, DMD, Periodontist and Implant Surgeon
Prosthetic Options After Surgery
Once your implant has integrated, the restorative phase begins. The type of prosthesis depends on how many teeth you are replacing and your functional goals:
- Single Crown: A porcelain or zirconia crown cemented or screwed onto a single implant. This is the most common restoration and feels indistinguishable from a natural tooth.
- Implant-Supported Bridge: Two or more implants support a multi-unit bridge, eliminating the need to grind down adjacent healthy teeth as with a traditional dental bridge.
- Full-Arch Fixed Prosthesis (All-on-4 / All-on-6): A complete set of teeth permanently attached to four to six implants. Often delivered as a same-day temporary prosthesis, with the final version fabricated after healing.
- Implant-Retained Overdenture: A removable denture that clips onto two to four implants for dramatically improved stability compared to conventional dentures.
FAQ: Your Questions About Implant Surgery Answered
The surgery itself is painless because the area is fully numbed with local anesthesia. Most patients describe the post-operative discomfort as mild to moderate -- comparable to or less than a tooth extraction. Over-the-counter ibuprofen or acetaminophen is usually sufficient to manage any soreness for the first 2-3 days.
A single implant placement typically takes 30-60 minutes of chair time. Multiple implants, bone grafting, or sinus lifts extend the appointment. Full-arch All-on-4 surgery usually requires 2-3 hours. The total treatment timeline from start to final crown delivery is typically 4-7 months.
For the first 1-2 weeks, you should stick to a soft-food diet -- soups, yogurt, scrambled eggs, mashed potatoes, and smoothies. Avoid hot, spicy, crunchy, or hard foods that could irritate the surgical site. Most patients return to their normal diet within 2-3 weeks, though you should avoid chewing directly on the implant until your surgeon confirms osseointegration.
Implant failure, while uncommon (2-4% of cases), is not the end of the road. The failed implant is removed -- a simple procedure since it has not bonded to the bone -- and the site is allowed to heal for 2-3 months. A new implant can then be placed, often with a bone graft to improve the site. Second-attempt success rates exceed 90%. Many surgeons include a warranty that covers the cost of one re-placement.
Look for a provider who has placed at least several hundred implants, uses CBCT imaging for every case, and can show before-and-after photos of similar cases. Periodontists, oral surgeons, and prosthodontists receive the most extensive implant training. Ask about the implant brand they use -- reputable manufacturers like Straumann, Nobel Biocare, and Zimmer Biomet offer decades of clinical data and universal part availability.
Sources
- Clinical Oral Implants Research. "Guided vs. Freehand Implant Placement: A Systematic Review and Meta-Analysis of Outcomes." Vol. 37, No. 2, 2026.
- International Journal of Oral & Maxillofacial Surgery. "Platelet-Rich Fibrin in Bone Augmentation: A Multicenter Randomized Trial." 2025.
- American Association of Oral and Maxillofacial Surgeons. "Parameters of Care: Clinical Practice Guidelines for Oral and Maxillofacial Surgery." 6th Ed., 2026.
- Journal of Periodontology. "Peri-implantitis: Prevalence, Risk Factors, and Treatment Outcomes -- A 2026 Update." Vol. 97, No. 3.
- National Association of Dental Plans. "Employer-Sponsored Dental Benefits Report." 2026.
- American Dental Association. "Guidelines for the Use of Sedation and General Anesthesia by Dentists." Updated January 2026.
