Contents
Dental Insurance Pre-Authorization in 2026: How to Get Procedures Approved and Avoid Denied Claims
Few aspects of dental insurance frustrate patients more than having a recommended procedure delayed or denied because the insurance company has not yet approved it. Pre-authorization -- also called prior authorization -- is the process through which your insurer reviews and approves a proposed treatment before it is performed. In 2026, this gatekeeping mechanism affects an estimated 35% of all dental claims above $300, making it a routine part of the patient experience for anything beyond preventive care.
Understanding how pre-authorization works, what triggers it, and how to navigate denials gives you a meaningful advantage. Patients who actively participate in this process alongside their dental providers are significantly more likely to receive timely approvals, avoid surprise bills, and secure the full benefits their plan offers.
What Is Dental Pre-Authorization and Why It Matters
Pre-authorization is a formal review process in which your dental insurance company evaluates a proposed treatment to determine whether it meets the plan's criteria for medical necessity and coverage. When your dentist recommends a crown, implant, or orthodontic treatment, the insurer wants to verify three things before committing to pay:
- Is the procedure medically necessary? The clinical evidence must support the need for the specific treatment recommended.
- Is the procedure covered under this specific plan? Even medically necessary treatments may be excluded by certain plan designs.
- Are there frequency or age limitations that apply? Many plans restrict how often a procedure can be performed (e.g., one crown per tooth every five years).
For patients, a successful pre-authorization provides critical financial certainty. It is a written commitment from your insurer that they will cover the procedure at the stated benefit level, assuming the treatment is performed as described. Without pre-authorization on procedures that require it, you risk having the entire claim denied after the fact -- leaving you responsible for the full cost.
Why Pre-Authorization Protects You
Think of pre-authorization as a binding estimate. Once approved, the insurer has committed to paying their share as long as the treatment matches what was submitted. This protects you from the costly scenario of receiving treatment and then discovering weeks later that your claim has been denied.
Pre-Authorization vs. Predetermination: Key Differences
These two terms are frequently confused, but they carry very different implications for your coverage and financial planning.
| Feature | Pre-Authorization (Prior Authorization) | Predetermination (Pre-Treatment Estimate) |
|---|---|---|
| Required? | Mandatory for specified procedures | Voluntary -- patient or provider choice |
| Guarantee of Payment? | Yes, when approved and conditions are met | No -- it is an estimate only |
| Consequence of Skipping | Claim may be denied entirely | No penalty -- treatment proceeds normally |
| Processing Time | 5--15 business days (regulated timelines) | 10--30 business days |
| Who Initiates? | Dental provider (required) | Dental provider or patient (optional) |
| Validity Period | 60--90 days from approval date | 60--90 days (varies by insurer) |
Critical Distinction
A predetermination is helpful for planning purposes, but it does not guarantee payment. Your insurer can still deny or reduce the claim when it is actually submitted after treatment. A pre-authorization, on the other hand, functions as a binding approval -- the insurer must honor it as long as the treatment performed matches the approved plan.
Procedures That Typically Require Pre-Authorization
While requirements vary by carrier and plan tier, the following categories of treatment almost universally require pre-authorization in 2026:
- Crowns and onlays: Porcelain, ceramic, and gold crowns -- typically the most frequently pre-authorized procedure
- Fixed bridges: Any multi-unit bridge replacing one or more missing teeth
- Dental implants: Including the implant fixture, abutment, and implant-supported crown
- Orthodontic treatment: Braces and clear aligner therapy for both children and adults
- Periodontal surgery: Scaling and root planing (deep cleaning), osseous surgery, and gum grafts
- Dentures and partials: Complete dentures, partial dentures, and relines
- Complex extractions: Surgical extraction of impacted wisdom teeth
- Sleep apnea appliances: Mandibular advancement devices prescribed for obstructive sleep apnea
- Treatment plans exceeding a dollar threshold: Some plans require pre-authorization for any treatment plan totaling more than $300--$500
Preventive services (cleanings, exams, routine X-rays) and most basic restorative procedures (simple fillings, simple extractions) typically do not require pre-authorization.
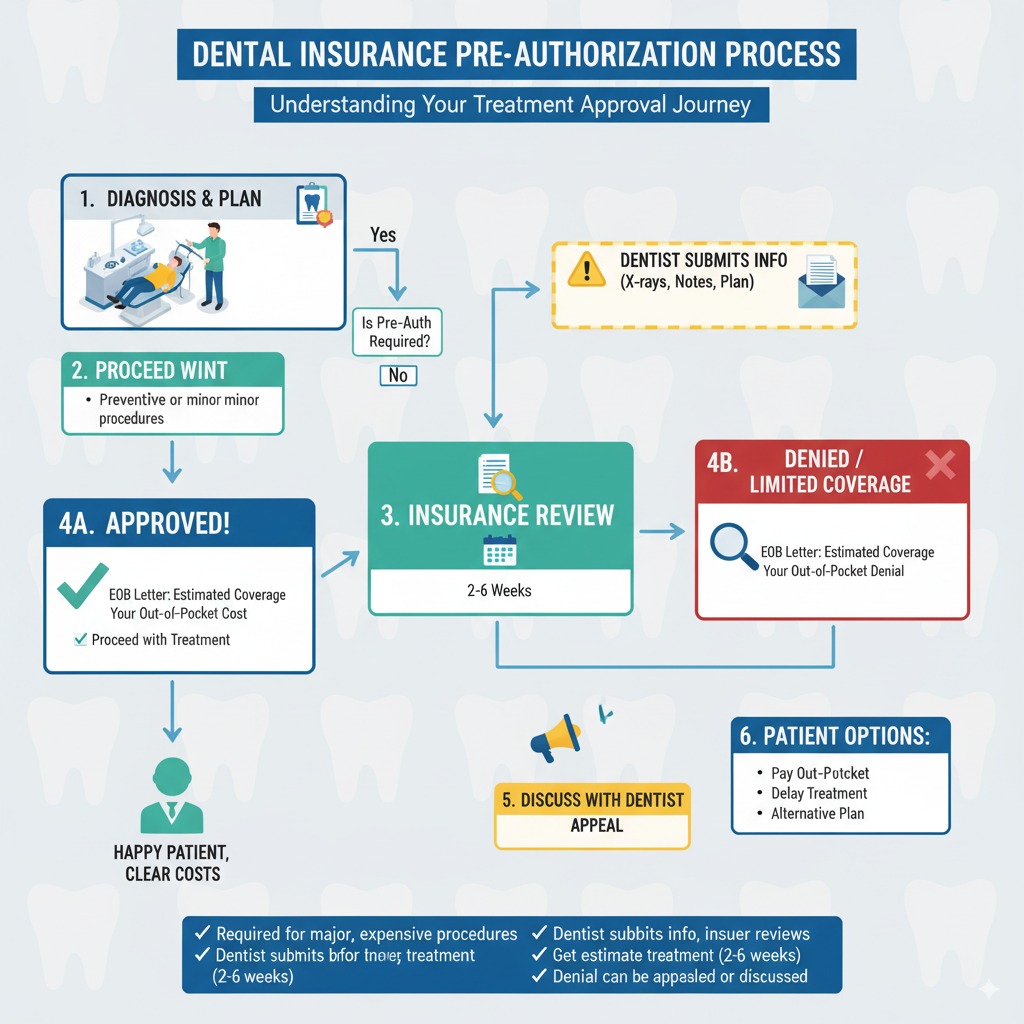
The Pre-Authorization Process Step by Step
The pre-authorization workflow is primarily managed by your dental office, but understanding each step helps you stay informed and proactive.
- Clinical examination and diagnosis. Your dentist examines the area, takes diagnostic records (X-rays, photographs, impressions or digital scans), and determines the recommended treatment.
- Treatment plan documentation. The dental office prepares a detailed submission including CDT procedure codes, narrative clinical notes explaining why the treatment is necessary, and all supporting diagnostic images.
- Electronic submission. In 2026, over 90% of pre-authorization requests are submitted electronically through clearinghouses or directly through insurer portals. Paper submissions are still accepted but take significantly longer to process.
- Insurance review. A clinical reviewer -- typically a licensed dentist employed by the insurance company -- evaluates the submission against the plan's coverage criteria, clinical guidelines, and frequency limitations.
- Decision issued. The insurer returns one of three outcomes: approved (the procedure is authorized at the stated benefit level), denied (with a specific reason code and explanation), or pended (additional information is needed before a decision can be made).
- Patient notification. Your dental office receives the decision and communicates it to you, including your estimated out-of-pocket cost if approved.
2026 Regulatory Changes Affecting Prior Authorization
The CMS Interoperability and Prior Authorization Final Rule, which began phased implementation in 2026, has introduced several important changes that affect dental plans offered through the ACA marketplace and Medicare Advantage programs:
- Faster decision timelines: Standard pre-authorization decisions must now be issued within 7 calendar days (reduced from 14). Urgent requests must be processed within 72 hours.
- Specific denial reasons required: Insurers must provide the specific clinical rationale for any denial, not just a generic reason code.
- Electronic exchange mandated: Plans must support fully electronic prior authorization transactions using the HIPAA X12 278 standard.
- Public reporting of approval rates: Insurers must now publicly report their prior authorization approval rates, denial rates, and average processing times.
"The new CMS transparency requirements are a game-changer for dental practices and patients alike. For the first time, we can compare insurers' approval rates side by side. This data gives dental offices leverage when choosing which plans to participate with, and gives patients meaningful information when selecting a plan during open enrollment."
-- Dr. Sarah Delgado, DDS, MBA, Dental Practice Management Consultant
Common Denial Reasons and How to Prevent Them
According to ADA Health Policy Institute data, approximately 12% of dental pre-authorization requests are initially denied. The most common reasons -- and how to prevent each one -- are detailed below.
| Denial Reason | Frequency | Prevention Strategy |
|---|---|---|
| Insufficient documentation | 35% of denials | Submit high-resolution X-rays, intraoral photos, and detailed narrative notes |
| Least Expensive Alternative Treatment (LEAT) clause | 25% of denials | Document why the alternative is clinically inadequate for this specific case |
| Frequency limitation not met | 18% of denials | Check the plan's frequency schedule before submitting; include documentation of prior treatment dates |
| Procedure not covered under plan | 12% of denials | Verify plan coverage and exclusions before treatment planning |
| Administrative errors (wrong codes, patient info) | 10% of denials | Double-check CDT codes, patient ID numbers, and provider NPI before submission |
The LEAT Clause: What You Need to Know
The Least Expensive Alternative Treatment clause is one of the most misunderstood provisions in dental insurance. When invoked, the insurer agrees to pay for a procedure -- but only up to the cost of a less expensive alternative that they deem clinically acceptable. For example, your plan may authorize a crown but only pay the equivalent cost of a large composite filling. The difference comes out of your pocket. Your dentist can help challenge LEAT decisions by documenting why the more expensive treatment is clinically superior for your specific condition.
How to Appeal a Denied Pre-Authorization
A denial is not the end of the road. In fact, appealing denied dental claims has a remarkably high success rate. Data from CMS and multiple state insurance commissioners shows that approximately 60--80% of appealed dental claim denials are partially or fully overturned. The appeal process typically follows this path:
- Review the denial notice carefully. The notice must state the specific reason for denial, the clinical criteria used, and your appeal rights. In 2026, insurers are required to provide this information in plain language.
- Gather additional clinical evidence. Your dentist should prepare supplemental documentation: higher-quality images, additional clinical measurements, periodontal charting, or peer-reviewed literature supporting the recommended treatment.
- Submit a formal written appeal. Most plans require appeals within 30--60 days of the denial date. The appeal should include a cover letter from your dentist, the supplemental evidence, and any relevant patient impact statement.
- Request a peer-to-peer review. Your dentist can request a direct conversation with the insurance company's reviewing dentist. This peer-to-peer discussion is often the most effective step in overturning a denial.
- Escalate to an external review if needed. If the internal appeal is denied, many states offer an external review process through an independent third party. This is your final administrative option before considering legal action.
"The single most effective action in any appeal is the peer-to-peer call. When my clinical team can speak directly with the insurer's reviewing dentist and walk through the radiographs, the patient's history, and the rationale for our treatment plan, the overturn rate jumps dramatically. Patients should always ask their dentist to pursue this option."
-- Dr. Michael Torres, DDS, FAGD, Director of Clinical Operations at a multi-location dental group
Do Not Delay Your Appeal
Most dental plans impose a strict deadline for filing appeals -- typically 30 to 60 days from the date of the denial notice. Missing this window usually means forfeiting your right to appeal. If you receive a denial, contact your dental office immediately to begin the process.
Patient vs. Provider Responsibilities
Pre-authorization is a collaborative process. Here is a clear breakdown of who is responsible for what:
Your dental provider's responsibilities:
- Determining which procedures require pre-authorization under your plan
- Preparing and submitting the clinical documentation package
- Following up with the insurer on pending requests
- Managing the appeals process if the initial request is denied
- Communicating the decision and estimated costs to you
Your responsibilities as a patient:
- Providing your current, accurate insurance information (ID card, group number, subscriber details)
- Understanding your plan's basic rules -- waiting periods, exclusions, annual maximums
- Asking your dental office whether pre-authorization is needed before scheduling major treatment
- Responding promptly if the insurer contacts you directly for additional information
- Requesting a copy of the approval or denial for your records
Expert Strategies for Faster Approvals
Dental offices that consistently achieve high approval rates and fast turnaround times share several best practices:
- Submit comprehensive documentation upfront. Include all required records in the initial submission rather than waiting for the insurer to request additional information. A complete first submission reduces processing time by an average of 8 business days.
- Use the correct CDT codes. Coding errors are the most easily preventable cause of denials. Ensure your dental team is trained on the latest CDT code updates (the 2026 code set includes 16 new codes and 12 revised codes).
- Write a strong narrative. The clinical narrative should explicitly connect the patient's symptoms, diagnostic findings, and treatment rationale. Generic narratives like "tooth needs crown" are insufficient; instead, document "tooth #14 exhibits a mesial-lingual cusp fracture extending below the CEJ with symptoms of irreversible pulpitis, rendering a direct restoration inadequate."
- Verify benefits before submitting. Call the insurer's provider line to confirm the patient's eligibility, remaining benefits, frequency limitations, and whether the specific procedure requires pre-authorization. This five-minute call prevents many common denial scenarios.
- Track and follow up systematically. Use your practice management software to flag outstanding pre-authorizations. If a decision has not been received within the regulatory timeline (7 days for standard requests), contact the insurer to escalate.
Conclusion: Mastering the Pre-Authorization Process
Pre-authorization is not going away -- if anything, it is becoming more standardized and more prevalent as insurers apply cost-management tools across a wider range of procedures. But the 2026 regulatory environment is more patient-friendly than ever: faster decision timelines, mandatory transparency in denial reasons, and public reporting of approval rates all give patients and providers more leverage and information.
The key takeaway is that pre-authorization is not an obstacle to overcome but a tool to use in your favor. When done correctly, it provides financial certainty, prevents billing surprises, and ensures that your insurance pays the maximum benefit available. Partner closely with your dental team, ask questions early, and never accept a denial without exploring the appeal process. The data consistently shows that persistence pays off.
FAQ: Dental Pre-Authorization Questions
Under the 2026 CMS Interoperability rule, standard pre-authorization decisions for applicable plans must be issued within 7 calendar days. Urgent requests must be processed within 72 hours. Commercial plans not subject to CMS rules may take 10--15 business days. Electronic submissions are consistently processed faster than paper submissions.
If pre-authorization was required for the procedure and you proceed without it, the insurer can deny the claim entirely. This means you would be responsible for the full cost of treatment. Some plans may still process the claim after the fact, but benefits may be reduced (typically by 20--50%). Always confirm whether pre-authorization is required before scheduling major dental work.
No. Insurance companies do not require pre-authorization for genuine dental emergencies, including acute infections, uncontrolled bleeding, traumatic injuries, and severe pain requiring immediate intervention. However, any non-emergency follow-up treatment (such as a permanent crown after an emergency buildup, or an implant after an emergency extraction) will likely require pre-authorization through the standard process.
Most pre-authorization approvals are valid for 60 to 90 days from the date of approval. If you do not receive the approved treatment within that window, you will need to submit a new pre-authorization request. Some insurers allow extensions if the patient can demonstrate a valid reason for the delay. Check the approval letter for the specific expiration date.
While some insurers technically allow patients to initiate requests, effective pre-authorization submissions require clinical documentation -- diagnostic X-rays, CDT procedure codes, and clinical narratives -- that only a dental provider can generate. In practice, pre-authorization is always handled by your dental office. Your role is to provide accurate insurance information and follow up on the status of the request.
Sources
- Centers for Medicare and Medicaid Services, "CMS Interoperability and Prior Authorization Final Rule (CMS-0057-F)," 2024
- American Dental Association, Health Policy Institute, "Prior Authorization in Dental Insurance: Trends and Impact on Access to Care," 2025
- National Association of Dental Plans, "Prior Authorization Practices in Commercial Dental Plans," 2025 Survey Report
- American Medical Association, "2025 Prior Authorization Physician Survey," 2025 (dental section)
- U.S. Department of Health and Human Services, "Patient Rights Under the Affordable Care Act: Appeals and Grievances," 2025 Update
- CDT 2026: Current Dental Terminology, American Dental Association, 2025
