Contents
Dental Insurance Waiting Periods in 2026: How They Work, How to Avoid Them & Smart Workarounds
You have just enrolled in a new dental insurance plan, eager to address that crown your dentist recommended six months ago. Then you read the fine print: there is a 12-month waiting period for major services. For the next year, you will pay premiums every month but receive zero coverage for the procedure you need most. This scenario plays out for millions of Americans each year, and it is one of the most frustrating aspects of individual dental insurance.
In 2026, waiting periods remain a standard feature of nearly every individual dental plan sold on the open market. Understanding exactly how they work, which plan types impose them, and what strategies can help you avoid or minimize them is essential for anyone purchasing dental insurance outside of an employer group.
What Are Dental Waiting Periods and Why Do They Exist?
A waiting period is a mandatory enrollment duration that must pass before your dental insurance plan will cover specific categories of treatment. During this time, you pay your monthly premiums but cannot access benefits for the procedures subject to the waiting period. If you receive one of those procedures during the waiting period, the plan will not reimburse any portion of the cost.
Waiting periods exist to prevent a practice insurers call adverse selection -- when individuals purchase insurance only after they know they need expensive treatment, collect the benefit, and then cancel coverage. Without waiting periods, this behavior would dramatically increase costs for the insurer, which would in turn drive up premiums for all members. Waiting periods ensure that the risk pool includes long-term members who pay premiums over time, not just people seeking a one-time payout.
The Key Distinction: Individual vs. Group Plans
Waiting periods are primarily a feature of individual dental plans purchased directly from an insurer or through the marketplace. Employer-sponsored group plans typically waive all waiting periods, offering full benefits from day one of enrollment. This is one of the most significant advantages of employer-provided dental insurance and a major reason group plans are generally the best value for dental coverage.
Waiting Periods by Service Category
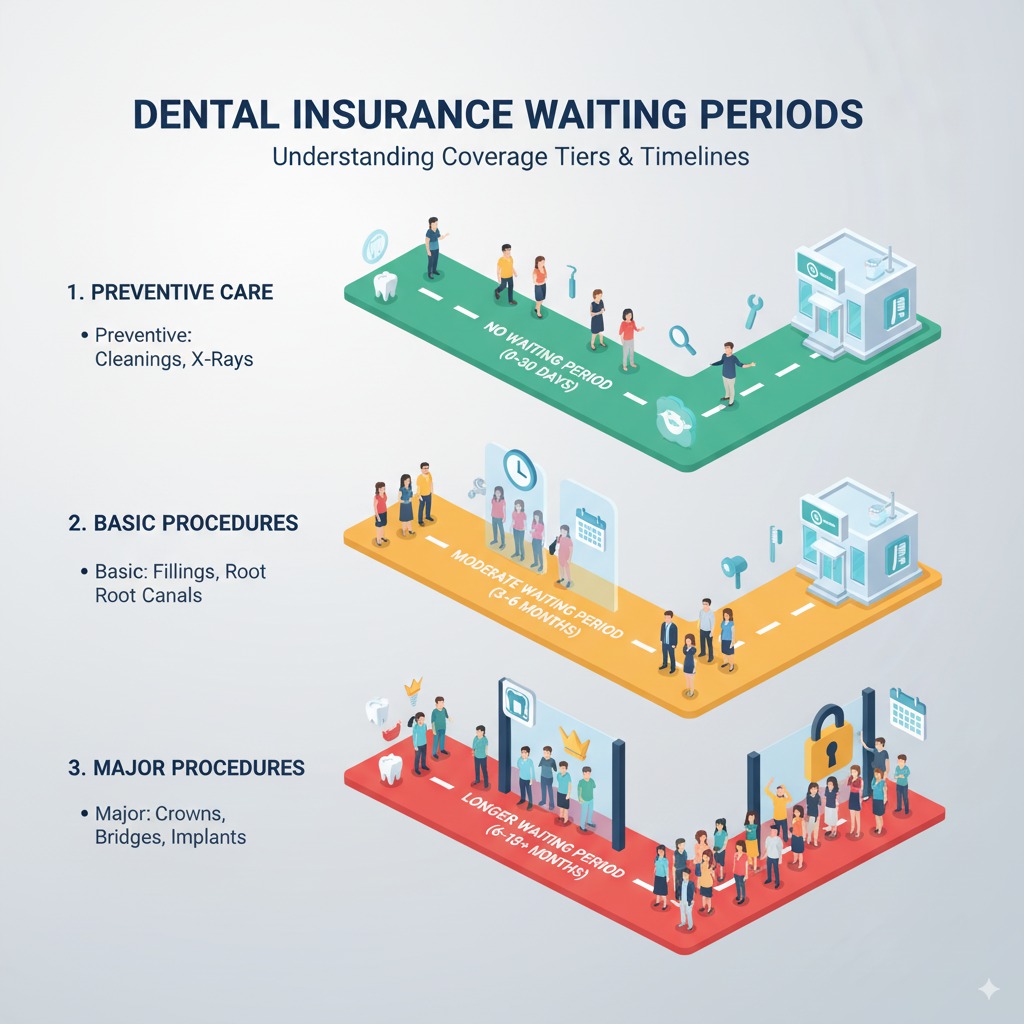
Dental insurance plans divide procedures into tiers, and each tier carries its own waiting period. The more expensive the service category, the longer the wait.
Preventive Care: Day One Coverage
Almost every dental plan -- individual or group -- covers preventive services immediately with no waiting period. This includes:
- Routine cleanings (prophylaxis) -- typically two per year
- Comprehensive and periodic oral exams
- Bitewing and panoramic X-rays
- Fluoride treatments for children
- Dental sealants for children
Insurers cover preventive care immediately because early detection and maintenance reduce the need for costly restorative and surgical procedures downstream.
Basic Services: 3 to 6-Month Wait
Basic restorative services typically carry a 3-to-6-month waiting period on individual plans. This tier includes:
- Composite and amalgam fillings
- Simple (non-surgical) tooth extractions
- Periodontal scaling and root planing (deep cleaning)
- Emergency palliative treatment
- Root canals on anterior teeth (some plans classify these as major)
Major Services: 6 to 12-Month Wait
Major dental services have the longest standard waiting periods, typically 6 to 12 months. These are the most expensive procedures:
- Porcelain and ceramic crowns
- Fixed bridges
- Complete and partial dentures
- Dental implants (fixture, abutment, and crown)
- Molar root canals
- Periodontal surgery and bone grafts
Orthodontics: 12 to 24-Month Wait
Orthodontic benefits -- for braces and clear aligners -- carry the longest waiting periods of any dental service category, often 12 to 24 months on individual plans. Some plans do not cover orthodontics at all. Employer-sponsored group plans that include orthodontic benefits usually waive the waiting period entirely.
| Service Category | Typical Coverage % | Individual Plan Wait | Employer Group Plan Wait |
|---|---|---|---|
| Preventive | 100% | None (Day 1) | None |
| Basic Restorative | 80% | 3--6 months | None |
| Major Services | 50% | 6--12 months | None |
| Orthodontics | 50% | 12--24 months | None |
Comparing Waiting Periods Across Major Carriers
Waiting period lengths vary by carrier and plan tier. The following comparison reflects 2026 individual plan offerings from major dental insurers. Group plan waiting periods are not included because they are almost universally waived.
| Carrier | Preventive Wait | Basic Wait | Major Wait | Ortho Wait |
|---|---|---|---|---|
| Delta Dental (Individual PPO) | None | 6 months | 12 months | 12 months |
| Cigna Dental (Individual) | None | 3 months | 12 months | 24 months |
| Humana Preventive Plus | None | 6 months | 12 months | Not covered |
| Guardian Direct | None | 3 months | 6 months | 12 months |
| Anthem Blue Cross (Individual) | None | 6 months | 12 months | 18 months |
| Spirit Dental (No-Wait Plan) | None | None | None | Not covered |
"Waiting periods are the single biggest surprise for people purchasing individual dental insurance. They see a plan with a $35 monthly premium and assume they can get a crown next month. When they discover there is a 12-month wait, they feel misled -- but it was always in the plan documents. My advice: read the waiting period schedule before anything else when evaluating a dental plan."
-- Lisa Chen, Licensed Insurance Broker, National Association of Health Underwriters
Plans with No Waiting Periods in 2026
While waiting periods are standard on individual plans, several options can give you faster access to benefits:
- Employer-sponsored group plans: The most reliable path to no waiting periods. Group plans pool risk across a large employee base, eliminating the adverse selection problem that drives individual plan waiting periods.
- Dental HMO (DHMO) plans: Most DHMO plans offer coverage from day one with no waiting periods for any service category. The trade-off is a restricted provider network and the requirement to select a primary care dentist.
- No-wait individual PPO plans: A small number of carriers (such as Spirit Dental and Denali Dental) offer individual PPO plans with no waiting periods. These plans typically compensate with higher premiums, lower annual maximums, or reduced coverage percentages for the first year.
- Dental discount plans: Not insurance, but membership programs that provide immediate access to discounted fees (typically 20--50% off) at participating providers. No waiting periods, no annual maximums, and no deductibles. Annual membership fees range from $80--$200 per individual.
No-Wait Plans: Read the Fine Print
Plans that advertise "no waiting periods" often compensate with lower annual maximums (sometimes as low as $1,000 in the first year), reduced coverage percentages during the first 12 months, or higher monthly premiums. Run the total-cost math: premiums + expected out-of-pocket costs for the year. A no-wait plan is not automatically the best value -- it depends on your specific treatment needs and timeline.
10 Strategies to Minimize or Avoid Waiting Periods
If you are purchasing an individual dental plan, these strategies can help you reduce the impact of waiting periods on your access to care:
- Enroll early. If you anticipate needing a crown, bridge, or other major work in 2027, enroll in a plan by January 2026 to start the waiting period clock immediately. The 12-month wait will end just as you are ready for treatment.
- Maintain continuous coverage. Many insurers will waive or credit waiting periods if you can demonstrate continuous prior dental coverage with no gap longer than 63 days. This is called a "creditable coverage" waiver and is one of the most valuable provisions in dental insurance.
- Ask about waiver policies when switching plans. Not all carriers honor creditable coverage from all prior insurers. When shopping for a new plan, specifically ask: "Will you waive waiting periods if I provide proof of prior continuous coverage?"
- Choose an employer plan when available. If you have access to an employer-sponsored dental plan, it is almost always superior to an individual plan for the simple reason that waiting periods are waived.
- Consider a DHMO for immediate coverage. If waiting periods are a dealbreaker and a DHMO is available in your area, the day-one coverage may outweigh the restricted network limitations.
- Use preventive benefits immediately. While waiting for basic and major coverage to activate, take full advantage of your day-one preventive benefits. Schedule a cleaning and comprehensive exam so your dentist can identify all issues and create a treatment plan timed to your waiting period schedule.
- Negotiate cash pricing during the wait. For urgent treatment needed during a waiting period, ask your dentist about a cash-pay discount. Many practices offer 10--20% off for patients paying out of pocket at the time of service.
- Stack a dental discount plan during the wait. Enroll in a dental discount plan (annual fee: $80--$200) to access reduced fees at participating providers while your insurance waiting period is active. Cancel the discount plan once your insurance benefits become available.
- Prioritize treatment based on waiting period timelines. Work with your dentist to address the most urgent issues first (often covered under basic services with shorter waits) and schedule major work for after the full waiting period has elapsed.
- Open enrollment timing. Individual dental plans purchased during the ACA open enrollment period (typically November through mid-January) begin coverage on January 1 or the first of the following month. If you enroll in November for a January 1 start date, your 12-month major services waiting period would end December 31 of the same year.
"The creditable coverage waiver is the most underutilized tool in dental insurance. I have seen patients who maintained continuous coverage for years but never thought to ask about a waiver when switching plans. They unnecessarily waited 12 months for benefits they could have had from day one. Always carry proof of your prior coverage dates and ask every new insurer about their waiver policy."
-- David Rothwell, CFP, Healthcare Benefits Advisor
Missing Tooth Clauses and Pre-Existing Conditions
Closely related to waiting periods are two other provisions that can limit your coverage for pre-existing dental conditions:
Missing Tooth Clause: Many dental plans include a "missing tooth clause" that excludes coverage for replacing a tooth that was already missing before your plan's effective date. If you lost a tooth in 2024 and enrolled in a plan in 2026, the plan may refuse to cover an implant or bridge to replace that tooth -- even after the waiting period has passed. Some plans do not have this clause, so it is an important factor to check when shopping for coverage.
Pre-Existing Condition Limitations: Unlike medical insurance, dental insurance is not subject to the ACA's prohibition on pre-existing condition exclusions. Dental plans can and do limit coverage for conditions that existed before enrollment. A cavity that was already present when you enrolled may not be covered for a filling during the basic services waiting period -- and in some cases, may trigger additional scrutiny even after the waiting period ends.
Emergency Treatment During Waiting Periods
Most plans make exceptions for genuine dental emergencies, even during active waiting periods. Emergency palliative treatment to relieve acute pain, control infection, or address traumatic injuries is typically covered regardless of waiting period status. However, the follow-up definitive treatment (permanent crown, implant, bridge) will still be subject to the waiting period for that service category.
How to Read Your Plan Documents
Before enrolling in any dental plan, locate and read these specific sections of the plan documentation:
- Summary of Benefits and Coverage (SBC): This standardized document lists covered services, coverage percentages, and -- critically -- waiting periods by service category. Look for a table or section labeled "Waiting Periods" or "Benefit Eligibility."
- Exclusions and Limitations: This section lists what the plan does not cover. Look for missing tooth clauses, pre-existing condition limitations, and any age-based restrictions.
- Creditable Coverage Policy: Check whether the plan offers waiting period waivers for members with prior continuous dental coverage. If this is not mentioned in the plan documents, call the insurer directly to ask.
- Frequency Limitations: Even after waiting periods expire, procedures are subject to frequency limits (e.g., one crown per tooth every 5 years). Understanding these limits prevents unpleasant surprises.
Conclusion: Planning Around Waiting Periods
Dental insurance waiting periods are a structural feature of individual plans that is unlikely to disappear anytime soon. They serve a legitimate actuarial purpose, and as long as individual dental plans are sold separately from medical insurance, insurers will continue to use waiting periods to manage risk and control costs.
The patients who navigate waiting periods most effectively are those who plan ahead. They enroll in coverage well before they expect to need major work, maintain continuous coverage to qualify for creditable coverage waivers, use preventive benefits from day one, and strategically time their treatment around waiting period expirations. By combining these approaches with alternative payment options like dental discount plans, HSA/FSA accounts, and negotiated cash pricing, you can ensure access to the care you need even when waiting periods are in effect.
FAQ: Dental Insurance Waiting Period Questions
Waiting periods protect the insurance pool from adverse selection -- the risk that individuals will purchase coverage only when they know they need expensive treatment and then cancel afterward. Without waiting periods, this behavior would make individual dental insurance financially unsustainable, driving premiums much higher for everyone. The premiums you pay during the waiting period fund the overall risk pool and ensure your coverage will be available when you need it.
A waiting period is a measure of time -- the number of months you must be enrolled before coverage for a service category activates. A deductible is a measure of money -- the dollar amount you must pay out of pocket each year before the insurance plan begins paying its share. They are separate requirements. After your waiting period expires, you still need to meet your annual deductible before the plan's coinsurance kicks in for basic and major services.
Not necessarily. Many dental insurers offer a creditable coverage waiver that eliminates or reduces waiting periods if you can demonstrate continuous prior dental coverage with no gap longer than 63 days. You will typically need to provide a certificate of coverage or letter from your previous insurer showing your enrollment dates. Ask the new insurer about their creditable coverage policy before enrolling, as not all carriers offer this benefit or accept all prior coverage types.
Most DHMO plans do not have waiting periods for any service category, including major procedures and orthodontics. This is one of the primary advantages of the DHMO model. However, DHMO plans require you to use an assigned in-network primary care dentist, have smaller networks, and require specialist referrals. Coverage is also limited to the plan's geographic service area, which makes DHMOs impractical for people who travel frequently or live in areas with limited DHMO availability.
Yes, most dental plans cover emergency palliative treatment regardless of waiting period status. This includes care to relieve acute pain, treat infections, and address traumatic injuries. However, the definitive follow-up treatment -- such as a permanent crown, implant, or root canal -- will still be subject to the waiting period for that service category. For example, if you crack a tooth during your waiting period, the plan may cover a temporary restoration for pain relief but will not cover the permanent crown until the major services waiting period expires.
Sources
- National Association of Dental Plans, "Individual Dental Plan Market Report: Waiting Periods and Plan Design," 2025
- American Dental Association, Health Policy Institute, "Dental Insurance Coverage Trends in the United States," 2025
- Delta Dental Plans Association, "2026 Individual Plan Summary of Benefits -- Waiting Period Schedules," January 2026
- Centers for Medicare and Medicaid Services, "Essential Health Benefits: Pediatric Dental Coverage Under the ACA," 2025 Update
- National Association of Insurance Commissioners, "Consumer Guide to Dental Insurance," 2025 Edition
- U.S. Department of Labor, Employee Benefits Security Administration, "Understanding Your Dental Benefits," 2025
