Contents
Dental Resin in 2026: Types, Applications, Durability, and How to Make It Last
Dental resin, officially known as composite resin, is the most widely used restorative material in modern dentistry. From filling cavities and bonding chipped teeth to crafting full composite veneers, this tooth-colored material has largely replaced silver amalgam as the standard of care. But how long does it actually last? What factors determine its durability? And how have recent material science advances changed the picture in 2026?
This in-depth guide answers these questions and more, providing the latest evidence on resin lifespan, expert insights, cost data, and practical strategies for ensuring your resin restorations last as long as possible.
What Is Dental Resin? Composition and Properties
Composite resin is a sophisticated engineered material consisting of three primary components that work together to produce a strong, aesthetic, and biocompatible restoration.
The Three Components
- Resin Matrix: The organic polymer base, typically Bis-GMA (bisphenol A-glycidyl methacrylate) or UDMA (urethane dimethacrylate). This is the "glue" that holds everything together and gives the material its moldable, paste-like consistency before curing.
- Filler Particles: Inorganic particles of glass, quartz, silica, or zirconia that provide strength, wear resistance, and opacity. The size and distribution of these particles determine the composite's classification (hybrid, nanofill, microfill) and its clinical properties.
- Coupling Agent: A silane-based chemical that bonds the filler particles to the resin matrix, ensuring the material behaves as a unified whole under stress.
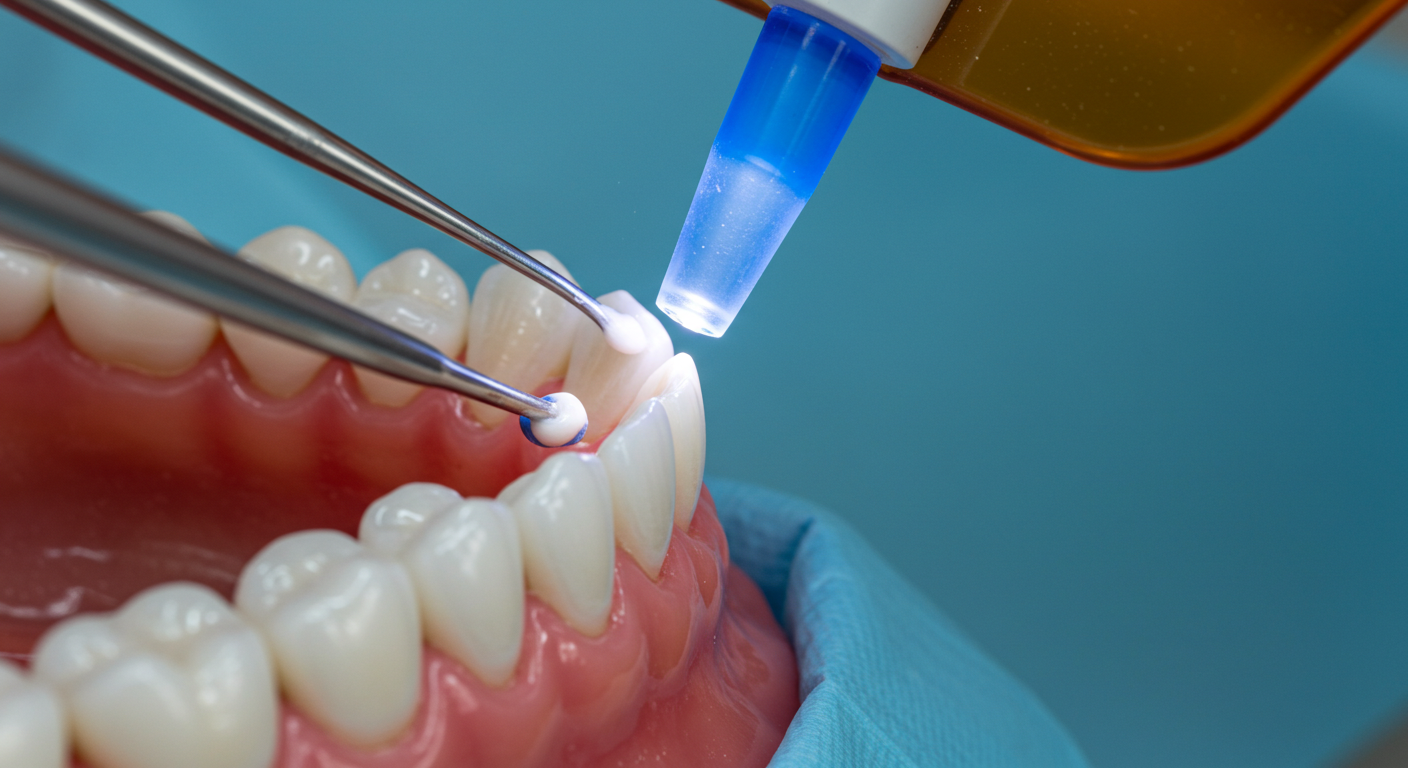
When your dentist applies the composite and shines a blue curing light on it, the light activates photoinitiators in the resin that trigger polymerization, hardening the material in seconds. This ability to cure on demand is what makes chairside resin restorations so efficient.
Dr. Anna Kowalski, DDS, PhD, Dental Materials Researcher: "The composite resins of 2026 are vastly superior to those from even a decade ago. Nano-hybrid formulations with sub-100-nanometer filler particles achieve a level of polish retention and wear resistance that was previously only possible with ceramics. We are genuinely closing the gap between resin and porcelain in many clinical situations."
The Six Major Applications of Dental Resin
Dental resin's versatility makes it the most multi-purpose material in the dental toolkit. Here are its six primary clinical applications in 2026.
| Application | Description | Typical Lifespan |
|---|---|---|
| Cavity Fillings | Replaces decayed tooth structure in both front and back teeth | 7-12 years |
| Cosmetic Bonding | Repairs chips, closes gaps, reshapes teeth | 5-8 years |
| Composite Veneers | Full coverage of the front surface of teeth for smile makeovers | 5-7 years |
| Core Buildups | Rebuilds tooth structure to support a crown after root canal | Matches crown lifespan |
| Sealants | Thin protective coating on the grooves of back teeth to prevent decay | 3-5 years |
| Temporary Restorations | Short-term restorations while a permanent prosthesis is fabricated | Weeks to months |
Composite Resin vs. Other Filling Materials
Patients often ask how composite resin compares to other filling materials. This side-by-side comparison reflects the current evidence in 2026.
| Feature | Composite Resin | Silver Amalgam | Ceramic Inlay/Onlay |
|---|---|---|---|
| Aesthetics | Excellent (tooth-colored) | Poor (silver/dark) | Excellent (tooth-colored) |
| Tooth Preservation | Conservative (bonds to tooth) | Requires more removal (mechanical retention) | Moderate (requires some preparation) |
| Average Lifespan | 7-12 years | 10-15 years | 15-25 years |
| Repairability | Easily repairable chairside | Must be fully replaced | Difficult to repair; usually replaced |
| Cost (2026) | $200 - $500 | $150 - $350 | $800 - $2,000 |
| Mercury Content | None | Contains approximately 50% mercury | None |
How Long Does Dental Resin Last? The 2026 Evidence
The durability of composite resin has improved significantly over the past two decades. Here is what the latest clinical research tells us.
- Small to Medium Fillings (1-2 surfaces): Average lifespan of 10-15 years with modern materials. A 2025 meta-analysis in Dental Materials found annual failure rates of 1.5-2.5% for posterior composites, meaning 85-90% of fillings survive beyond 10 years.
- Large Fillings (3+ surfaces): Average lifespan of 5-8 years. Larger restorations are subjected to greater stress and have more margin length susceptible to decay and fracture.
- Anterior (Front Teeth) Restorations: Average lifespan of 8-12 years. These experience lower biting forces but are more prone to staining and edge chipping.
- Composite Veneers: Average lifespan of 5-7 years. More susceptible to staining and chipping than porcelain veneers but can be easily repaired or replaced.
Dr. Marcus Wei, DDS, FAGD: "The biggest predictor of how long a composite filling will last is not the material itself--it is the patient's habits and hygiene. I have placed composite fillings that lasted 18 years in patients with excellent oral care, and I have seen them fail in under two years in patients who grind their teeth without a nightguard or neglect brushing."
Factors That Shorten or Extend Resin Lifespan
Understanding what affects resin durability empowers you to take protective action.
Factors That Shorten Lifespan
- Bruxism (Teeth Grinding): Generates forces up to 600 psi on restorations, causing micro-cracks, fractures, and accelerated wear. A custom nightguard is essential for bruxism patients.
- Poor Oral Hygiene: Plaque accumulation at the margins of the restoration leads to secondary (recurrent) caries, which is the number one reason composite fillings fail.
- High-Sugar/High-Acid Diet: Frequent sugar exposure feeds decay-causing bacteria, while acidic beverages (citrus, soda, sports drinks) can soften the resin surface over time.
- Large Restoration Size: The bigger the filling, the more stress it absorbs and the more margin area is exposed to potential breakdown.
- Staining Habits: Coffee, tea, red wine, and tobacco cause surface discoloration. While this does not affect structural integrity, it can make the restoration visually unacceptable, prompting earlier replacement.
Factors That Extend Lifespan
- Excellent Oral Hygiene: Brushing twice daily with fluoride toothpaste and daily flossing prevent decay at the restoration margins.
- Regular Dental Visits: Professional cleanings every 6 months and periodic polishing of composite surfaces maintain the finish and allow early detection of problems.
- Using a Nightguard: Protects restorations from bruxism forces during sleep.
- Rubber Dam Isolation: When the dentist places the composite under rubber dam isolation, the bond quality is significantly better because moisture contamination is eliminated.
The Latest Advances in Resin Technology
Composite resin technology continues to evolve rapidly. Here are the most significant developments reshaping the field in 2026.
- Bulk-Fill Composites: These can be placed in layers up to 4-5 mm thick (versus the traditional 2 mm), reducing chairtime and the number of increments needed. Studies show comparable long-term performance to conventional layered composites.
- Self-Healing Composites: Experimental resins containing encapsulated healing agents that activate when micro-cracks form, sealing damage before it propagates. Early clinical trials show promising results.
- Bioactive Composites: Formulations that release fluoride, calcium, and phosphate ions to actively remineralize tooth structure at the restoration-tooth interface, reducing the risk of secondary caries.
- 3D-Printed Resin Restorations: Digital workflows now allow dentists to 3D-print highly accurate composite inlays and onlays chairside, combining the convenience of direct restorations with the precision of lab-fabricated ones.
How to Maximize the Lifespan of Your Resin Restorations
Follow these evidence-based strategies to get the most years out of your composite restorations.
- Brush Twice Daily with Fluoride Toothpaste: Use a soft-bristled brush and non-abrasive toothpaste. Avoid whitening toothpastes with high abrasivity (RDA above 100), as they can scratch and dull composite surfaces.
- Floss Daily: Floss prevents decay at the contact points between teeth--a common area for secondary caries around fillings.
- Limit Staining Beverages: Drink coffee, tea, and red wine through a straw when possible, and rinse with water afterward. Avoid tobacco in all forms.
- Avoid Biting Hard Objects: Do not chew ice, hard candy, popcorn kernels, or pen caps. These create point-loading forces that can fracture composite.
- Get a Custom Nightguard: If you clench or grind your teeth, a nightguard is one of the best investments you can make to protect both your natural teeth and your restorations.
- Schedule Professional Polishing: Ask your hygienist to polish your composite restorations with composite-specific polishing cups during your regular cleanings. This removes surface stains and restores the smooth finish that resists plaque accumulation.
- Address Issues Early: If you notice a rough edge, staining, or sensitivity around a filling, see your dentist promptly. Small repairs are quick and inexpensive; waiting until the restoration fails completely often means a larger, more expensive replacement.
Cost of Dental Resin Procedures in 2026
Composite resin procedures are among the most affordable in dentistry, especially relative to ceramic alternatives. Here are updated 2026 prices.
- Composite Filling (1 surface): $200 - $350
- Composite Filling (2 surfaces): $275 - $450
- Composite Filling (3+ surfaces): $350 - $550
- Cosmetic Bonding (per tooth): $300 - $700
- Composite Veneer (per tooth): $300 - $800
- Dental Sealant (per tooth): $40 - $80
Most dental insurance plans classify composite fillings as "basic" services, covered at 80% after the deductible. Cosmetic bonding and veneers may not be covered if deemed purely elective. Sealants are typically covered at 100% for children under 18.
Sources
- Leinfelder KF, et al. "Clinical performance of posterior composites: a 20-year retrospective analysis." Dental Materials. 2025;41(2):178-192.
- Demarco FF, et al. "Longevity of posterior composite restorations: not only a matter of materials." Dental Materials. 2024;40(1):e1-e21.
- American Dental Association. "2026 Survey of Dental Fees." ADA Health Policy Institute, 2026.
- Frontiers in Dental Medicine. "Bioactive and self-healing dental composites: current status and future prospects." 2025;6:article 1089234.
- National Institute of Dental and Craniofacial Research. "Dental Composite Restorations: What Patients Should Know." NIDCR, updated 2025.
FAQ: Your Top Questions About Dental Resin
No, composite resin does not respond to teeth whitening products (hydrogen peroxide or carbamide peroxide). If you whiten your natural teeth, existing composite fillings will retain their original shade and may become noticeably mismatched. The best approach is to whiten your teeth first, wait two weeks for the shade to stabilize, and then have your composite restorations replaced or repaired to match the new, lighter shade.
Composite resin is considered safe by the ADA, FDA, and major international health agencies. The Bis-GMA monomer used in many composites is derived from bisphenol A (BPA), but the amount of BPA that may leach from a cured composite filling is extremely small--less than what you would absorb from handling a receipt or eating canned food. Many modern composites now use BPA-free monomers (such as UDMA or TEGDMA) for patients who prefer to avoid any BPA exposure entirely. Discuss BPA-free options with your dentist if this is a concern.
Signs that a composite filling may need replacement include: sensitivity to hot, cold, or sweet foods; a visible dark line or gap around the edge of the filling; a rough or chipped surface you can feel with your tongue; visible staining that cannot be polished away; or detection of decay around the filling on an X-ray during a routine check-up. Your dentist will monitor the condition of your restorations at every visit and recommend replacement only when clinically necessary.
The ADA does not recommend replacing amalgam fillings solely because of concerns about mercury. If an amalgam filling is intact and functioning well, removing it unnecessarily removes additional healthy tooth structure and is not justified. However, if an amalgam filling is cracked, leaking, or has decay around it, replacing it with composite is an excellent choice. Many patients also choose replacement for purely aesthetic reasons, which is a valid personal decision. Discuss the pros and cons with your dentist for your specific situation.
Yes, repairability is one of composite resin's greatest advantages. If a small chip or fracture occurs, your dentist can roughen the existing surface, apply a bonding agent, and add new composite material directly. This repair can be done in a single appointment, costs less than a full replacement, and preserves more tooth structure. However, if the damage is extensive, secondary decay is present, or the bond has broken down around the margins, a full replacement is the better option.
