Contents
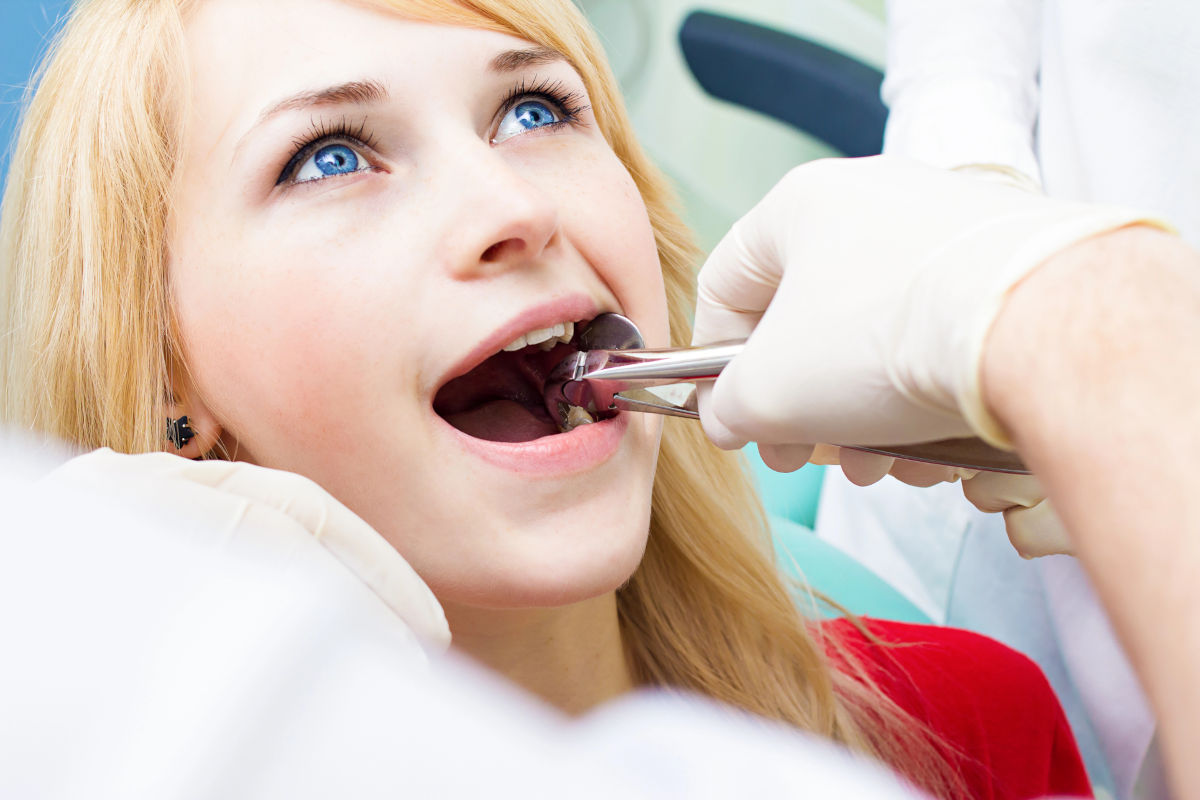
Tooth Extraction Procedure: Complete 2026 Guide to Types, Recovery, and Cost
Having a tooth pulled is one of the most common dental procedures in the United States, with approximately 15 million extractions performed annually according to the American Association of Oral and Maxillofacial Surgeons. Despite its frequency, the prospect of an extraction can be daunting for many patients. The good news is that modern dentistry in 2026 has refined the procedure to be safer, faster, and more comfortable than ever before. Whether you are facing a simple extraction of a loose tooth or a complex surgical removal of an impacted wisdom tooth, this comprehensive guide covers every aspect of the process, from preparation through full recovery.
Quick Facts About Tooth Extraction in 2026
A simple extraction typically takes 20-40 minutes from start to finish. Modern local anesthetics ensure the procedure is painless. Most patients return to normal activities within 2-3 days. The extraction socket fully heals with new bone in approximately 3-4 months.
When Is a Tooth Extraction Medically Necessary?
Dentists always prioritize saving a natural tooth whenever possible. Extraction is recommended only when preservation through fillings, crowns, or root canal therapy is no longer viable. The following situations commonly necessitate extraction in 2026.
- Severe Tooth Decay: When decay has destroyed so much of the tooth structure that no restorative material can reliably rebuild it, the tooth must be removed to prevent infection of the jawbone.
- Advanced Periodontal Disease: Stage III or Stage IV periodontitis can erode the bone and ligaments anchoring the tooth, leading to excessive mobility that makes the tooth non-functional.
- Dental Abscess or Infection: When a periapical or periodontal abscess cannot be resolved with antibiotics and root canal treatment, extraction prevents the infection from spreading to adjacent teeth or into the bloodstream.
- Impacted Wisdom Teeth: Third molars that are partially erupted, angled, or trapped beneath the gum often cause recurrent infections, cysts, or damage to neighboring second molars.
- Orthodontic Treatment: Planned extractions of premolars may be necessary to create adequate space for orthodontic alignment, particularly in cases of severe crowding.
- Fractured Roots: A tooth that has cracked vertically through the root cannot be saved and must be extracted to prevent infection and bone loss.
"A tooth extraction is never our first choice, it is our last resort. But when a tooth is beyond saving, removing it promptly protects the patient's overall oral health and opens the door to effective replacement options." -- Dr. Sarah Mitchell, Oral Surgery Fellow, NYU Langone Dental Medicine, 2025
Simple vs. Surgical Extraction: Types Explained
The two fundamental categories of tooth extraction differ in complexity, technique, and recovery time. Understanding which type applies to your situation helps set appropriate expectations.
| Feature | Simple Extraction | Surgical Extraction |
|---|---|---|
| When Performed | Tooth is fully visible and accessible above the gum line | Tooth is impacted, broken below the gum, or has complex root anatomy |
| Who Performs It | General dentist | Oral surgeon or general dentist with surgical training |
| Anesthesia | Local anesthetic only | Local anesthetic, often with IV sedation or general anesthesia |
| Incision Required | No | Yes (gum flap raised, bone may be removed) |
| Procedure Time | 20-40 minutes | 45-90 minutes |
| Recovery Time | 2-3 days | 5-10 days |
| Stitches | Rarely needed | Usually required (often dissolvable) |
In a simple extraction, the dentist uses an instrument called an elevator to gently loosen the tooth from its periodontal ligament, then grasps it with forceps and removes it with a controlled rocking motion. The entire process typically takes just a few minutes once the area is numb.
A surgical extraction is more involved. The surgeon makes an incision in the gum tissue to create a flap, exposing the tooth and surrounding bone. In some cases, a small amount of bone overlying the tooth must be removed with a surgical handpiece. For large or multi-rooted teeth, the surgeon may section the tooth into smaller pieces for easier removal. The site is then cleaned, and the gum flap is sutured closed.
The Extraction Procedure Step by Step
Knowing exactly what will happen during your appointment can significantly reduce anxiety. Here is the standard protocol followed by most dental offices in 2026.
- Pre-Operative Assessment: Your dentist reviews your medical history, current medications, and any allergies. A periapical or panoramic X-ray (or a cone-beam CT scan for complex cases) is taken to evaluate root anatomy, proximity to nerves, and the condition of surrounding bone.
- Anesthesia Administration: A topical numbing gel is applied to the injection site, followed by local anesthetic injection. You will feel a brief pinch, then complete numbness within 3-5 minutes. Sedation is administered at this stage if applicable.
- Tooth Loosening: The dentist places an elevator instrument between the tooth and surrounding bone, applying controlled force to sever the periodontal ligament fibers and rock the tooth within its socket.
- Tooth Removal: Once sufficiently loosened, dental forceps are used to grasp the crown of the tooth and extract it with a steady, firm pull combined with rotation.
- Socket Management: The socket is inspected and debrided of any granulation tissue or infection. If the bone walls are fractured, they are smoothed. In some cases, bone graft material is placed to preserve the ridge for future implant placement.
- Hemostasis: A sterile gauze pad is placed over the socket and you bite down firmly to promote blood clot formation. Sutures are placed if needed.
- Post-Op Instructions: You receive written aftercare instructions, prescriptions for pain management and antibiotics if indicated, and a follow-up appointment is scheduled.
Anesthesia and Sedation Options in 2026
One of the greatest advances in modern extraction procedures is the range of comfort options available to patients. Beyond standard local anesthesia, several sedation modalities can transform the experience for anxious patients.
- Local Anesthesia: The standard for all extractions. Agents such as articaine and lidocaine with epinephrine provide complete numbness for 2-4 hours. You remain fully awake and aware.
- Nitrous Oxide (Laughing Gas): Inhaled through a mask, nitrous oxide produces mild relaxation and reduces anxiety while you remain conscious. Its effects wear off within minutes of removing the mask, allowing most patients to drive themselves home.
- Oral Sedation: A benzodiazepine such as triazolam (Halcion) is taken by mouth 30-60 minutes before the procedure. You remain conscious but deeply relaxed and may have limited memory of the procedure. A driver is required.
- IV Sedation: Medications are delivered directly into the bloodstream for rapid, precisely controlled sedation. Commonly used for surgical extractions and multiple extractions. You will have little to no memory of the procedure.
- General Anesthesia: Reserved for complex surgical cases, pediatric patients, or individuals with special needs. Administered in an oral surgery office or hospital setting with an anesthesiologist.
Insurance Note
Most dental insurance plans cover local anesthesia as part of the extraction fee. Sedation options (nitrous oxide, oral sedation, IV sedation) are typically billed separately and may or may not be covered depending on your plan. Check with your insurance provider before the procedure to avoid unexpected out-of-pocket costs.
Tooth Extraction Cost and Insurance Coverage in 2026
The cost of a tooth extraction in the United States varies based on the type of extraction, geographic location, and whether sedation is used. Below are the current average costs as of early 2026.
| Procedure Type | Cost Without Insurance | Typical Insurance Coverage | Estimated Out-of-Pocket |
|---|---|---|---|
| Simple Extraction | $150 - $450 | 70-80% after deductible | $30 - $135 |
| Surgical Extraction (erupted tooth) | $300 - $650 | 50-80% after deductible | $60 - $325 |
| Impacted Wisdom Tooth (soft tissue) | $350 - $700 | 50-80% after deductible | $70 - $350 |
| Impacted Wisdom Tooth (bony) | $500 - $1,100 | 50-80% after deductible | $100 - $550 |
| All 4 Wisdom Teeth (surgical) | $1,500 - $3,500 | 50-80% after deductible | $300 - $1,750 |
Most PPO and DHMO dental insurance plans classify simple extractions as a "basic" procedure (covered at 70-80%) and surgical extractions as a "major" procedure (covered at 50-80%). Annual maximums of $1,000 to $2,500 apply, which is an important consideration if you need multiple extractions. Patients without insurance can often negotiate cash-pay discounts of 10-20% or set up payment plans through third-party financing companies like CareCredit or Sunbit.
Post-Extraction Recovery Timeline and Aftercare
Following your dentist's aftercare instructions closely is the single most important factor in preventing complications and ensuring smooth healing.
Critical Warning: Protect the Blood Clot
The blood clot that forms in the extraction socket is essential for healing. Dislodging it leads to a painful condition called dry socket. For the first 24 hours after extraction, do NOT smoke, spit forcefully, use a straw, rinse your mouth vigorously, or consume hot liquids. These actions create suction or pressure that can pull the clot out of the socket.
First 24 Hours: Bite on gauze for 30-45 minutes after the procedure. Apply an ice pack to the outside of your cheek (20 minutes on, 20 minutes off) to minimize swelling. Eat only soft, cool foods such as yogurt, applesauce, or smoothies (no straw). Take prescribed pain medication before the anesthesia wears off. Rest with your head elevated.
Days 2-3: Swelling typically peaks 48-72 hours after extraction. Begin gently rinsing your mouth with warm saltwater (1/2 teaspoon of salt in 8 ounces of warm water) after meals. You can gradually introduce semi-soft foods like scrambled eggs, mashed potatoes, and pasta. Continue taking pain medication as needed.
Days 4-7: Swelling should begin to subside. Discomfort transitions from aching to mild soreness. Most patients can resume normal activities including work and light exercise. If dissolvable sutures were placed, they begin to dissolve around day 5-7.
Weeks 2-4: The gum tissue closes over the socket. You can return to a normal diet, though you may still want to chew on the opposite side. Non-dissolvable sutures, if used, are removed at your follow-up appointment around day 7-10.
Months 2-4: New bone gradually fills the extraction socket. The ridge may appear slightly concave compared to the pre-extraction contour, which is normal bone remodeling.
"The number one cause of post-extraction complications I see is patients resuming smoking too soon. Even one cigarette within the first 72 hours dramatically increases the risk of dry socket. The chemicals in smoke impair blood flow and inhibit clot stability." -- Dr. James Rivera, DDS, Oral and Maxillofacial Surgeon, 2026
Risks, Complications, and Warning Signs
While tooth extraction is a safe and routine procedure, being aware of potential complications allows you to respond promptly if they arise.
- Dry Socket (Alveolar Osteitis): Occurs in 2-5% of extractions (up to 30% for impacted lower wisdom teeth). Symptoms include severe, radiating pain starting 2-4 days post-extraction, a visible empty socket without a clot, and a foul taste. Treatment involves irrigation and placement of a medicated dressing by your dentist.
- Infection: Characterized by worsening pain, increasing swelling, fever, pus discharge, and a foul taste. Usually treated with antibiotics. Report any fever above 101 degrees F to your dentist immediately.
- Excessive Bleeding: Some oozing is normal for 24-48 hours. If active bleeding soaks through gauze within an hour, or if you are spitting out large clots, contact your dentist.
- Nerve Injury: A rare complication (less than 1%) primarily associated with lower wisdom teeth. The inferior alveolar nerve or lingual nerve can be bruised during extraction, causing temporary numbness or tingling of the lip, chin, tongue, or gums. Permanent nerve damage is extremely rare.
- Sinus Communication: When extracting upper molars, a small opening between the mouth and the maxillary sinus can occur. This usually heals on its own with precautions (avoiding blowing your nose, sneezing with your mouth open) but occasionally requires surgical closure.
When to Call Your Dentist Immediately
Seek urgent care if you experience: uncontrollable bleeding that does not stop with firm gauze pressure after 30 minutes; fever above 101 degrees F; severe pain that worsens after 3-4 days instead of improving; difficulty breathing or swallowing; or numbness that has not begun to resolve after 8 hours.
Tooth Replacement Options After Extraction
Unless the extracted tooth is a wisdom tooth, replacing it is strongly recommended. Leaving a gap allows adjacent teeth to drift, opposing teeth to over-erupt, and bone to resorb, all of which can compromise your bite and facial aesthetics over time.
- Dental Implant: A titanium post is surgically placed in the jawbone and topped with a custom crown. Implants are the gold standard for tooth replacement, offering the most natural look, feel, and function. Healing time is 3-6 months. Learn more about dental implants.
- Dental Bridge: A fixed prosthesis that uses the teeth on either side of the gap as anchors for a pontic (false tooth). A bridge is completed in 2-3 appointments and does not require surgery, but it does require reducing healthy adjacent teeth.
- Removable Partial Denture: A cost-effective, non-surgical option consisting of replacement teeth attached to a gum-colored base. It is removable for cleaning and may feel less stable than fixed options.
- Immediate Implant Placement: In select cases, an implant can be placed into the socket at the same appointment as the extraction. This approach reduces overall treatment time and preserves bone volume, but requires favorable anatomy and an infection-free extraction site.
Timing Matters
If you plan to get a dental implant but are not doing immediate placement, ask your dentist about socket preservation (bone grafting at the time of extraction). Without it, the jawbone can lose up to 50% of its width within the first year, potentially making future implant placement more difficult or requiring additional bone grafting procedures.
Sources
- American Association of Oral and Maxillofacial Surgeons. Parameters for Tooth Extraction, Clinical Practice Guidelines, 2024
- Bouloux GF, Steed MB, Perciaccante VJ. Complications of third molar surgery. Oral and Maxillofacial Surgery Clinics of North America, 2007 (cited in 2025 meta-analysis)
- Kolokythas A, Olech E, Miloro M. Alveolar osteitis: a comprehensive review of concepts and controversies. International Journal of Dentistry, 2010 (updated 2024)
- American Dental Association. Tooth Extraction: What to Expect. ADA MouthHealthy, 2025
- Anitua E, Alkhraisat MH. Socket preservation using bone grafting materials. European Journal of Oral Implantology, 2024
FAQ: Your Top Questions About Tooth Extraction in 2026
During the procedure itself, you should feel absolutely no pain. Modern local anesthetics completely numb the tooth, gum, and surrounding bone. You will feel pressure and possibly a pushing or rocking sensation, but these are not painful. After the anesthesia wears off, you can expect moderate soreness for 2-4 days, which is well managed with over-the-counter ibuprofen (400-600 mg every 6 hours) and acetaminophen (500-1000 mg every 6 hours), often taken in alternation. Your dentist will prescribe stronger medication only if needed.
For a simple extraction, most patients feel significantly better within 2-3 days and can return to normal activities. Surgical extractions, particularly impacted wisdom teeth, typically require 5-10 days of recovery before you feel comfortable. The soft tissue over the socket usually closes within 2-3 weeks, while the underlying bone takes 3-4 months to fully remodel and fill the socket. Complete healing varies by individual, age, and overall health.
For the first 24-48 hours, stick to soft, cool foods: yogurt, applesauce, smoothies (no straw), mashed potatoes, scrambled eggs, and lukewarm soup. Avoid hot foods and beverages, crunchy or hard foods, spicy foods, and anything with small seeds that could lodge in the socket. After 3-4 days, you can gradually reintroduce firmer foods. Most patients return to their normal diet within 7-10 days, chewing on the opposite side of the extraction until it is fully healed.
Yes, for any tooth other than a wisdom tooth, replacement is strongly recommended. A missing tooth causes adjacent teeth to shift toward the gap, the opposing tooth to over-erupt, and the jawbone beneath the gap to slowly resorb. Over time, these changes can affect your bite, jaw joint, speech, and facial appearance. The three main replacement options are dental implants (gold standard), fixed bridges, and removable partial dentures. Your dentist can help you choose the best option based on your anatomy, health, and budget.
Dry socket (alveolar osteitis) occurs when the blood clot in the extraction socket dissolves or is dislodged before healing is complete, exposing the underlying bone and nerves. It causes severe, throbbing pain that often radiates to the ear and a bad taste or odor from the socket. To prevent it: do not smoke for at least 72 hours (ideally longer), avoid using straws or spitting forcefully, do not rinse vigorously for 24 hours, eat soft foods, and follow all aftercare instructions. If you develop dry socket, your dentist will irrigate the socket and place a medicated dressing to relieve pain and promote healing.
