Contents
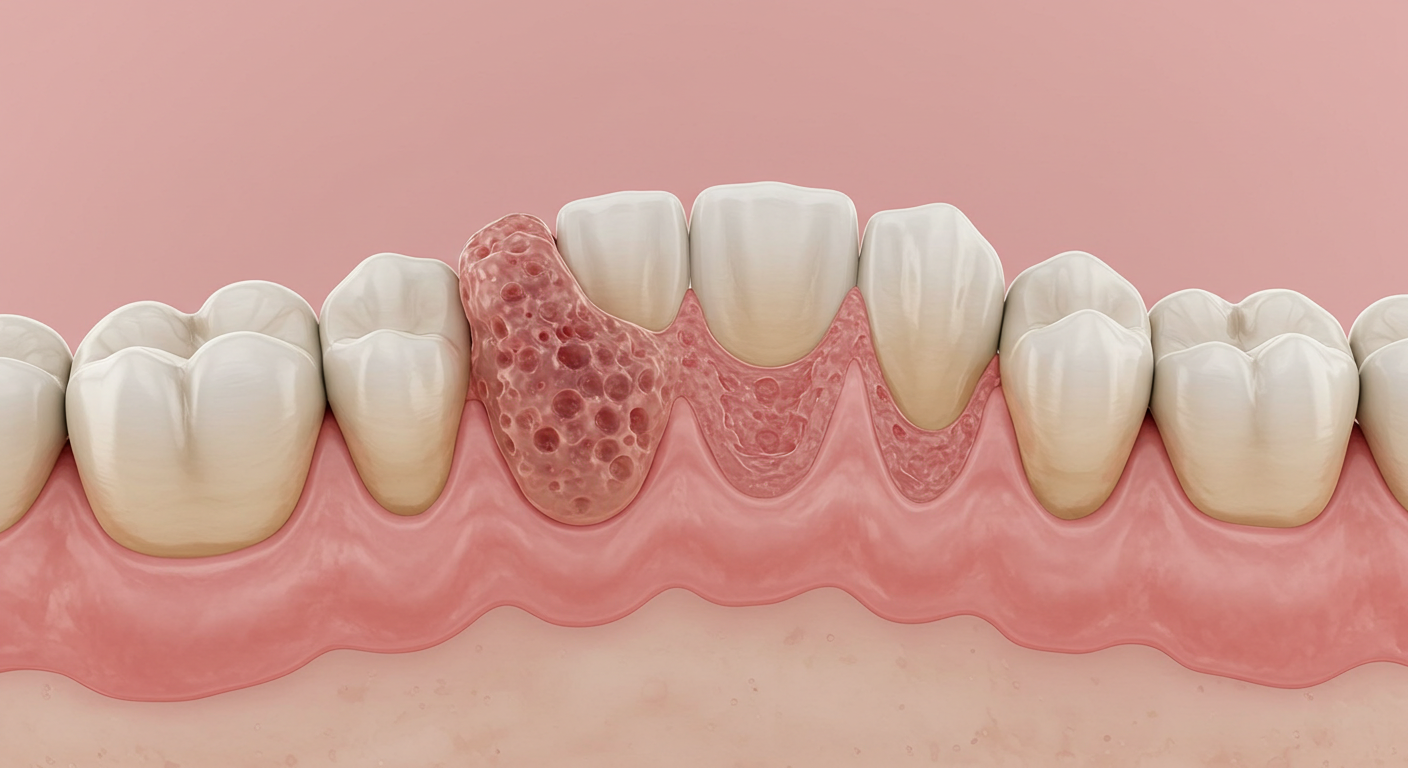
Dental Granuloma in 2026: Causes, Diagnosis, Treatment Options, and Long-Term Prognosis
A dental granuloma, also called a periapical granuloma, is one of the most common pathological findings in dental practice, yet it remains widely misunderstood by patients. This small, benign mass of chronic inflammatory tissue forms at the tip of a tooth's root as the body's attempt to contain a bacterial infection that has escaped from the tooth's interior. Because a granuloma can persist silently for months or even years without producing noticeable symptoms, many patients are surprised when their dentist discovers one on a routine X-ray and recommends treatment.
In this comprehensive 2026-updated guide, we cover the biology behind granuloma formation, how modern diagnostic imaging has improved detection, the full range of treatment options from conservative endodontics to surgical intervention, the critical differences between granulomas and related conditions like cysts and abscesses, and what happens when a granuloma is left untreated. Understanding this condition empowers you to make informed decisions about your dental care and avoid potentially serious complications.
What Is a Dental Granuloma and Why Does It Form?
A periapical granuloma is a localized mass of chronic granulomatous inflammatory tissue that develops at the apex (the very tip) of a tooth root. It is not a tumor and it is not cancerous. Instead, it represents the immune system's defensive barrier against bacteria that have escaped from the root canal system of a non-vital (dead) tooth into the surrounding periapical bone.
When the dental pulp, the living tissue inside a tooth containing nerves and blood vessels, dies due to decay, trauma, or other insults, the pulp chamber and root canals become colonized by bacteria. These microorganisms and their toxic byproducts gradually migrate through the apical foramen (the tiny opening at the root tip) into the surrounding jawbone. The immune system responds by dispatching macrophages, lymphocytes, plasma cells, and fibroblasts to the area. These cells form a compact mass of granulomatous tissue that walls off the infection and prevents it from spreading freely into the bone and adjacent structures.
"A periapical granuloma is essentially a biological stalemate. The immune system cannot eliminate the bacteria because they are sheltered inside the root canal, and the bacteria cannot overwhelm the immune barrier. This standoff can persist for years, silently destroying bone, until the equilibrium is broken." -- Dr. Hideaki Suda, Professor of Endodontology, Tokyo Medical and Dental University
On a dental radiograph, a granuloma typically appears as a well-defined radiolucent (dark) area surrounding the root apex, usually less than 10 millimeters in diameter. Larger lesions may represent the transition from granuloma to radicular cyst, though definitive differentiation requires histopathological examination of the tissue.
Key Fact: How Common Are Dental Granulomas?
Periapical granulomas account for approximately 75 percent of all periapical lesions found during endodontic surgery or extraction. Radicular cysts account for roughly 15 to 20 percent, and periapical abscesses make up the remaining 5 to 10 percent. Given that millions of root canal treatments are performed globally each year, granulomas represent one of the most frequently encountered pathological entities in dentistry.
Root Causes of Periapical Granulomas
The formation of a dental granuloma is always preceded by pulp necrosis (death of the tooth's internal tissue). The main pathways leading to pulp necrosis include:
Untreated Dental Caries
The most common cause. When tooth decay is allowed to progress unchecked, bacteria penetrate through the enamel and dentin and eventually reach the pulp chamber. The resulting pulpitis (inflammation of the pulp) can initially be reversible, but once infection is established, the pulp tissue undergoes irreversible necrosis. The bacteria then have a direct route through the root canals to the apex.
Dental Trauma
A blow to a tooth, whether from a sports injury, fall, or accident, can sever the blood supply entering through the apical foramen. Without blood flow, the pulp tissue dies even if the tooth appears externally intact and undamaged. This is why dentists recommend monitoring traumatized teeth with periodic vitality tests and radiographs for several years after an injury. A granuloma may not develop until months or years after the initial trauma.
Failed or Incomplete Root Canal Treatment
Root canal therapy has a high overall success rate (85 to 97 percent depending on the study and clinical context), but failures do occur. Common reasons include missed canals (many teeth have complex canal anatomy with accessory and lateral canals), inadequate disinfection, incomplete obturation (filling), or coronal leakage from a poor-quality final restoration. When residual bacteria persist or re-enter the canal system, a new granuloma can form at the apex.
Other Contributing Factors
- Cracked or fractured teeth: Cracks that extend to the pulp create pathways for bacterial invasion.
- Extensive dental procedures: Repeated restorative work on the same tooth (multiple fillings, crown preparations) can cumulatively irritate and damage the pulp.
- Periodontal disease: In advanced cases, bacteria from deep periodontal pockets can reach the root apex through lateral canals, creating a combined endodontic-periodontic lesion.
Symptoms and Clinical Signs to Watch For
One of the defining and most clinically significant characteristics of a dental granuloma is its ability to remain completely asymptomatic for extended periods. Because it represents a chronic, contained infection rather than an acute one, many patients carry a granuloma for years without any awareness of its presence. This is precisely why regular dental checkups with periodic radiographic screening are so important.
When symptoms do manifest, they tend to be subtle and intermittent:
- A dull, low-grade ache or sensation of pressure around the affected tooth.
- Mild discomfort when biting down or tapping the tooth (percussion sensitivity).
- A small, recurring pimple on the gum (sinus tract or fistula) that may intermittently drain pus. This is actually the body's pressure-relief mechanism and often keeps the infection from becoming acutely painful.
- Slight darkening or grayish discoloration of the affected tooth, indicating pulp necrosis.
- Localized gum swelling or tenderness directly over the root apex area.
- An unpleasant taste in the mouth if the fistula is actively draining.
Warning: Acute Flare-Ups Can Happen Without Warning
A chronic granuloma can transition to an acute periapical abscess at any time, particularly when the patient's immune system is compromised by illness, stress, or immunosuppressive medication. An acute flare-up presents with severe throbbing pain, facial swelling, fever, and potential difficulty swallowing or breathing. This is a dental emergency that requires immediate professional treatment.
Diagnosis: How Dentists Detect Granulomas in 2026
Modern dental diagnostics have significantly improved the detection and characterization of periapical lesions. The diagnostic workup for a suspected granuloma in 2026 typically includes a combination of clinical testing and advanced imaging.
Clinical Testing
The dentist will perform pulp vitality tests using cold stimulation (ethyl chloride or refrigerant spray) and electric pulp testing (EPT) to determine whether the tooth's pulp is alive or necrotic. A non-vital tooth that does not respond to these stimuli is the primary clinical indicator. Percussion testing (tapping the tooth) and palpation of the overlying gum tissue provide additional diagnostic information about the presence and extent of periapical inflammation.
Radiographic Imaging
| Imaging Modality | What It Shows | Advantages | Limitations |
|---|---|---|---|
| Periapical radiograph (2D) | Dark area at root tip; overall root and canal morphology | Low cost, low radiation, widely available | Superimposition of structures; cannot differentiate granuloma from cyst |
| CBCT (3D cone beam CT) | Three-dimensional view of lesion size, location, and relationship to adjacent structures | Precise spatial information; detects lesions missed on 2D films; invaluable for surgical planning | Higher cost and radiation dose than 2D; not always necessary for straightforward cases |
| AI-assisted radiograph analysis | Automated detection and measurement of periapical radiolucencies | Reduces missed diagnoses; standardizes interpretation; rapid screening of large image databases | Still requires clinician validation; variable accuracy across software platforms |
A notable advancement in 2026 is the increasing integration of artificial intelligence (AI) tools into dental radiograph interpretation. Several commercially available platforms now use deep learning algorithms to automatically flag periapical radiolucencies on panoramic and periapical radiographs, alerting the dentist to lesions that might otherwise be overlooked during visual assessment. While these tools do not replace the clinician's judgment, they serve as a valuable second set of eyes, particularly for detecting small or early-stage granulomas.
"The combination of CBCT imaging and AI-assisted analysis has fundamentally changed how we approach periapical pathology. We can now detect lesions earlier, plan surgeries more precisely, and monitor healing with greater objectivity than was possible even five years ago." -- Dr. Elena Konstantinova, Chair of Endodontics, Charite University Hospital Berlin, 2026
Treatment Options: From Conservative to Surgical
The primary goal of all granuloma treatment is identical: eliminate the bacterial source within the root canal system. Once the microorganisms and their toxic byproducts are removed, the body's immune system can resolve the granulomatous tissue and regenerate bone in the previously infected area. Treatment options are ordered from most conservative to most invasive.
Conventional Root Canal Treatment
This is the first-line and most common treatment for a tooth with a periapical granuloma that has not previously been endodontically treated. The procedure involves accessing the pulp chamber, locating all root canals (modern microscopy and CBCT guidance have significantly improved canal identification), meticulously cleaning and shaping the canals using rotary nickel-titanium instruments, irrigating with antimicrobial solutions (primarily sodium hypochlorite and EDTA), and finally obturating (filling) the disinfected canals with biocompatible materials. The tooth is then restored with a permanent filling or crown.
Success rates for primary root canal treatment in teeth with periapical lesions range from 85 to 95 percent in well-executed cases. Complete radiographic healing of the granuloma typically occurs within 6 to 24 months after treatment, though clinical symptoms usually resolve much sooner.
Endodontic Retreatment
When a previously root-canal-treated tooth develops a granuloma (indicating treatment failure), retreatment is the next conservative option. The clinician removes the existing root canal filling material, re-cleans and re-shapes the canals with particular attention to areas that may have been missed or inadequately treated the first time, re-disinfects, and places a new obturation. Retreatment success rates are generally lower than primary treatment (approximately 70 to 85 percent) because the canal anatomy may have been altered by the initial procedure and residual bacteria in biofilms can be more resistant to disinfection.
Apicoectomy and Microsurgical Endodontics
When conventional retreatment is not feasible (for example, due to a well-fitting post and core, calcified canals, or anatomical obstacles) or has failed, periapical microsurgery (apicoectomy) is the next option. Under local anesthesia, the endodontist makes a small incision in the gum, creates a window in the bone to access the root apex, curettes out the granuloma tissue, resects (cuts off) the last 3 millimeters of the root tip, and places a retrograde filling (typically using mineral trioxide aggregate or bioceramics) to seal the root canal from the apical end.
Modern microsurgical techniques using operating microscopes, ultrasonic root-end preparation tips, and bioceramic filling materials have elevated success rates for apicoectomy to approximately 90 to 95 percent in specialized hands. The granuloma tissue removed during surgery is routinely sent for histopathological examination to confirm the diagnosis and rule out other pathologies.
Tooth Extraction
Extraction is reserved as a last resort when the tooth cannot be saved due to extensive structural damage, a vertical root fracture, or failure of all other endodontic interventions. Removing the tooth eliminates the source of infection entirely, and the granuloma tissue is curetted from the socket at the time of extraction. The resulting gap should subsequently be managed with a prosthetic replacement such as a dental implant, fixed bridge, or removable partial denture to prevent the adjacent teeth from shifting and to restore function.
| Treatment | Success Rate | Typical Healing Time | When It Is Indicated |
|---|---|---|---|
| Primary root canal | 85 - 95% | 6 - 24 months | First-time treatment of non-vital tooth with granuloma |
| Endodontic retreatment | 70 - 85% | 6 - 24 months | Failed previous root canal |
| Apicoectomy (microsurgical) | 90 - 95% | 3 - 12 months | Failed retreatment or retreatment not feasible |
| Tooth extraction | 100% (infection eliminated) | 4 - 8 weeks (socket healing) | Non-restorable tooth or failed endodontic surgery |
Bioceramic Materials: A 2026 Game-Changer
The widespread adoption of bioceramic sealers and retrograde filling materials (such as EndoSequence BC Sealer and TotalFill BC RRM) has significantly improved outcomes in both conventional endodontics and apicoectomy. These calcium silicate-based materials are biocompatible, hydrophilic (they set in the presence of moisture), dimensionally stable, and have demonstrated the ability to promote cementum and bone regeneration at the root apex. Many endodontists now consider bioceramics the material of choice for root-end fillings.
Granuloma vs. Cyst vs. Abscess: Understanding the Differences
Patients and even some general practitioners sometimes confuse these three periapical conditions. While they are related and can evolve from one to another, they represent distinct pathological entities with different clinical behaviors and, in some cases, different treatment implications.
| Feature | Periapical Granuloma | Radicular (Periapical) Cyst | Periapical Abscess |
|---|---|---|---|
| Nature | Solid mass of chronic inflammatory tissue | Fluid-filled epithelial-lined cavity | Collection of pus (acute infection) |
| Symptoms | Usually asymptomatic | Usually asymptomatic; may cause displacement of adjacent teeth if large | Severe pain, swelling, fever |
| Radiographic appearance | Small radiolucency at root tip (typically less than 10 mm) | Well-defined radiolucency, often larger, with a corticated (sclerotic) border | Diffuse radiolucency or widened periodontal ligament space |
| Definitive diagnosis | Histopathology | Histopathology | Clinical presentation and aspiration |
| Response to root canal treatment | Usually heals completely | Smaller cysts may heal; larger true cysts may require surgical enucleation | Requires drainage plus root canal or extraction |
| Prevalence among periapical lesions | ~75% | ~15 - 20% | ~5 - 10% |
The key clinical distinction is that while most granulomas resolve with conventional root canal treatment alone, some radicular cysts (particularly larger "true cysts" that have become self-sustaining) may not respond to endodontic therapy and require surgical enucleation. This is why accurate diagnosis and follow-up imaging are essential.
Complications of Leaving a Granuloma Untreated
Although a dental granuloma is a benign lesion and a defensive mechanism, ignoring it carries substantial risks. The infection source within the root canal persists, and the clinical situation will inevitably deteriorate over time.
Warning: A Granuloma Will Not Resolve Without Treatment
No amount of antibiotics, mouthwash, or home remedies can eliminate a dental granuloma. Antibiotics can temporarily suppress acute symptoms, but they cannot reach effective concentrations inside the necrotic root canal where the bacteria reside. The only definitive cure is endodontic treatment or extraction of the affected tooth.
- Progression to a radicular cyst: Chronic inflammatory stimulation of epithelial cell rests of Malassez in the periodontal ligament can lead to cyst formation. Cysts cause greater bone destruction and may be more difficult to treat.
- Acute abscess formation: If the immune balance is disrupted (through stress, illness, or immunosuppression), the chronic granuloma can transform into an acute abscess with severe pain, pus accumulation, and facial swelling.
- Progressive bone loss: The chronic inflammatory process gradually resorbs surrounding alveolar bone. Extensive bone loss can compromise the structural support for adjacent teeth and make future implant placement more challenging, potentially requiring bone grafting procedures.
- Spread of infection to adjacent anatomical spaces: In rare but serious cases, untreated periapical infections can spread into the maxillary sinus (causing odontogenic sinusitis), the fascial spaces of the head and neck (causing cellulitis or Ludwig's angina), or, in extremely rare cases, enter the bloodstream (bacteremia).
- Potential systemic health implications: Research published between 2023 and 2025 continues to explore associations between chronic oral infections (including periapical lesions) and systemic conditions such as cardiovascular disease, diabetes complications, and adverse pregnancy outcomes. While causality is not definitively established, the association provides additional motivation for timely treatment.
Prevention and Long-Term Prognosis
The best strategy against dental granulomas is prevention, which centers on maintaining optimal oral health to prevent the pulp necrosis that triggers granuloma formation in the first place.
- Regular dental checkups: Biannual visits with periodic radiographic screening allow your dentist to detect cavities early, before they reach the pulp.
- Prompt treatment of cavities: A small filling today prevents a root canal tomorrow.
- Mouthguards for contact sports: Protecting teeth from trauma reduces the risk of pulp necrosis from dental injuries.
- Follow-up after trauma: Any tooth that has received a significant blow should be monitored with vitality tests and radiographs over the following one to five years.
- Quality restorative work: Ensuring crowns and fillings have proper margins that seal out bacteria protects the underlying tooth structure and reduces the risk of secondary decay reaching the pulp.
When properly treated with modern endodontic techniques, the long-term prognosis for a tooth with a periapical granuloma is excellent. The vast majority of granulomas heal completely after successful root canal treatment, with bone regeneration filling the previously radiolucent area within one to two years. Regular follow-up radiographs at 6 months, 12 months, and then annually for several years after treatment allow the clinician to confirm healing and detect any recurrence early.
"With modern instruments, irrigation protocols, bioceramic materials, and microscopic visualization, we can save teeth with periapical granulomas that would have been extracted a generation ago. The key is timely intervention before irreversible structural damage occurs." -- American Association of Endodontists, Clinical Practice Guidelines, 2025
Sources
- American Association of Endodontists. "Endodontic Diagnosis and Treatment Planning." AAE Clinical Practice Guidelines, 2025.
- Nair, P.N.R. "Pathogenesis of Apical Periodontitis and the Causes of Endodontic Failures." Critical Reviews in Oral Biology and Medicine, Vol. 15, No. 6, 2004.
- European Society of Endodontology. "Quality Guidelines for Endodontic Treatment." International Endodontic Journal, 2024.
- Setzer, F.C., et al. "Outcome of Endodontic Surgery: A Meta-Analysis of the Literature." Journal of Endodontics, 2024.
- Torabinejad, M., et al. "Mineral Trioxide Aggregate and Bioceramic Materials in Endodontics: A Review." Journal of Endodontics, 2025.
- FDI World Dental Federation. "Policy Statement on Retention of the Natural Dentition." 2024.
- Konstantinova, E. "AI-Assisted Radiograph Interpretation in Endodontic Diagnosis." European Journal of Dentistry, 2026.
FAQ: Dental Granulomas Explained
No. A dental granuloma cannot heal spontaneously because the source of infection, the bacteria colonizing the necrotic root canal inside the tooth, remains inaccessible to the immune system and to antibiotics. The granuloma will persist indefinitely and may grow larger or transform into a cyst or abscess over time. The only way to resolve a granuloma is to eliminate the bacterial source through root canal treatment or tooth extraction.
Absolutely not. Despite the name sounding similar to "granulomatous" conditions associated with other medical specialties, a periapical granuloma is a completely benign (non-cancerous) inflammatory reaction. It is composed of immune cells that are attempting to contain a localized bacterial infection. It does not metastasize, does not invade healthy tissue aggressively, and is not related to oral cancer in any way.
Clinical symptoms such as pain and sensitivity usually resolve within days to weeks after successful root canal treatment. However, complete radiographic healing, where the dark area on the X-ray fills in with new bone, typically takes 6 to 24 months. Your dentist will take follow-up radiographs at 6-month and 12-month intervals to confirm that healing is progressing normally. In some cases, a small scar-like area of fibrous tissue may remain visible on radiographs even after successful treatment, which is considered an acceptable outcome.
No. Antibiotics alone cannot cure a dental granuloma. While antibiotics may be prescribed as an adjunct to manage acute symptoms or prevent the spread of infection (particularly in cases of acute abscess flare-up or in medically compromised patients), they cannot penetrate the necrotic root canal space where the bacteria are harbored. Without mechanical removal of the infected tissue through root canal treatment, the infection will recur once the antibiotic course is completed. This is why endodontic treatment or extraction is always the definitive therapy.
A granuloma is a solid mass of chronic inflammatory tissue, while a cyst is a fluid-filled, epithelial-lined cavity that can develop from a long-standing granuloma. Granulomas account for about 75 percent of periapical lesions and generally respond well to root canal treatment alone. Cysts account for about 15 to 20 percent and may require surgical removal (enucleation) if they are large or if they have become self-sustaining "true cysts." The two conditions cannot be definitively distinguished on a standard radiograph alone; histopathological examination of the tissue is required for definitive diagnosis.
